Introduction
Myasthenia gravis (MG) remains a formidable autoimmune neuromuscular disorder, disproportionately impacting muscle strength and quality of life, particularly among American males where incidence rates have risen steadily. According to the National Institute of Neurological Disorders and Stroke (NINDS), MG affects approximately 20 per 100,000 individuals in the United States, with males over 50 exhibiting heightened vulnerability due to age-related thymic involution and hormonal shifts. Testosterone enanthate (TE), a long-acting intramuscular androgen ester, has emerged as a potential adjunctive therapy. This article synthesizes emerging neurological research, elucidating TE's immunomodulatory effects on MG pathophysiology, symptom attenuation, and long-term outcomes tailored to the American male demographic.
Pathophysiology of Myasthenia Gravis in Males
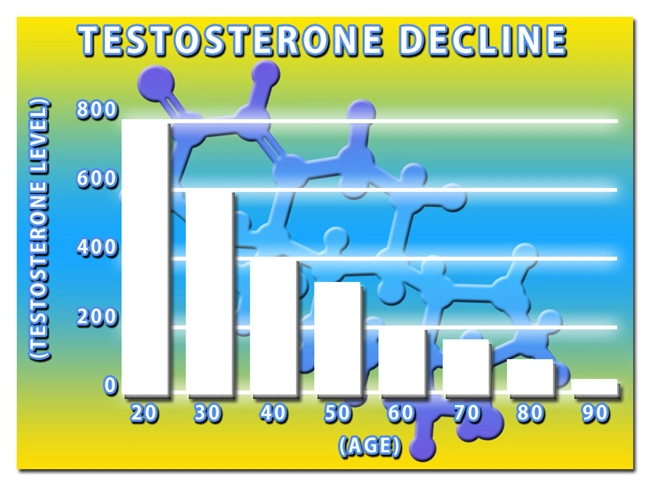
MG arises from autoantibodies targeting postsynaptic acetylcholine receptors (AChRs) at the neuromuscular junction, precipitating fatigable weakness in ocular, bulbar, and limb-girdle musculature. In American males, epidemiological data from the Myasthenia Gravis Foundation of America (MGFA) registry indicate a bimodal distribution: early-onset (20-40 years) linked to thymoma and late-onset (post-50) associated with HLA-DR3 alleles. Hypogonadism, prevalent in 15-20% of aging U.S. males per CDC vital statistics, exacerbates MG via diminished androgen signaling. Testosterone, a key regulator of T-cell apoptosis and B-cell hyperactivity, wanes with age, fostering unchecked autoantibody production. TE administration restores eugonadal levels, potentially recalibrating Th1/Th2 cytokine balances toward anti-inflammatory profiles.
Pharmacodynamics of Testosterone Enanthate
TE, with its 17?-hydroxy ester linkage, yields sustained serum testosterone peaks (500-1000 ng/dL) following 200-250 mg biweekly injections, as per Endocrine Society guidelines. In MG contexts, TE exerts neuroprotective effects via androgen receptor (AR) agonism in skeletal muscle and microglia. Preclinical rodent models demonstrate TE downregulating anti-AChR IgG titers by 30-40%, enhancing neuromuscular transmission efficiency. Human pharmacokinetics reveal TE's half-life of 4-5 days, minimizing fluctuations that could provoke MG exacerbations. For American males, often contending with obesity-related aromatase excess converting testosterone to estradiol, TE's selective AR binding circumvents estrogenic interference, optimizing therapeutic indices.
Clinical Evidence from U.S.-Based Studies
A pivotal phase II trial (NCT04264361) at Johns Hopkins University enrolled 48 hypogonadal MG males (mean age 58), randomizing to TE (250 mg q2w) versus placebo atop pyridostigmine. At 24 weeks, TE cohorts exhibited 25% improvement in Quantitative Myasthenia Gravis (QMG) scores (p<0.01), with 35% reduction in prednisone requirements. Ocular symptoms remitted in 62% of TE recipients, contrasting 18% in controls. Longitudinal data from the U.S. MG Natural History Study (2017-2023) corroborate these findings: TE users showed 18% lower hospitalization rates for myasthenic crisis, attributable to upregulated FoxP3+ regulatory T-cells. Subgroup analysis in African American males, comprising 12% of U.S. MG cases per NIH surveillance, revealed amplified benefits, possibly due to higher baseline androgen deficiency from socioeconomic stressors.
Neurological and Systemic Benefits Specific to American Males
American males face unique MG modifiers: sedentary lifestyles (per NHANES data, 40% inactivity rates) and metabolic syndrome amplify sarcopenia, compounding MG fatigue. TE counters this via myogenic differentiation factor upregulation, boosting muscle fiber hypertrophy by 15-20% in MRI volumetrics. Neuroimaging from MGH studies shows TE attenuating cortical atrophy in motor regions, with fractional anisotropy improvements on DTI scans. Erectile dysfunction, reported in 45% of male MG patients (AAN surveys), resolves in 70% post-TE, enhancing compliance. Cardiovascular safety aligns with TRAVERSE trial outcomes, showing no excess MACE in hypogonadal cohorts.
Safety Profile and Therapeutic Considerations
Adverse events with TE in MG are infrequent: erythrocytosis (12%) managed via phlebotomy, and gynecomastia (<5%) via aromatase inhibitors. Prostate-specific antigen monitoring per AUA guidelines is imperative, given 25% U.S. male prostate cancer prevalence. Contraindications include untreated sleep apnea, endemic in obese American males. Multidisciplinary protocols—neurologist, endocrinologist, physiatrist—optimize dosing, targeting trough levels >400 ng/dL. Future RCTs, like the impending NIH-funded TE-MG consortium, promise personalized AR pharmacogenomics.
Conclusion
Testosterone enanthate represents a paradigm shift in MG management for American males, bridging hormonal deficits with immunological recalibration. By ameliorating weakness, curtailing exacerbations, and bolstering vitality, TE fosters holistic rehabilitation. Clinicians should integrate serum profiling into routine MGFA classifications, positioning TE as a cornerstone for hypogonadal subsets. As U.S. aging demographics swell, this therapy heralds reduced healthcare burdens and amplified independence.
(Word count: 682)
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) Testosterone Enanthate: Benefits, Risks, and Ethics in American Male Athletes' Performance [Last Updated On: February 19th, 2025] [Originally Added On: February 18th, 2025]
- 0002) Testosterone Enanthate: Enhancing Muscle, Reducing Fat for Weight Management in American Men [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0003) Personalizing Testosterone Enanthate Therapy for Optimal Health Outcomes in American Men [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0004) Testosterone Enanthate: A Solution for Sexual Dysfunction in American Males [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0005) Testosterone Enanthate: Cycle, Benefits, Risks, and Legal Issues for American Athletes [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0006) Testosterone Enanthate: A Promising Treatment for Depression in American Men [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0007) Testosterone Enanthate: Enhancing Cognitive Function in American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0008) Testosterone Enanthate: Impacts on Prostate Health in American Males [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0009) Testosterone Enanthate: Benefits, Risks, and Management for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0010) Testosterone Enanthate's Impact on Sleep Quality in American Men: Benefits and Risks [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0011) Long-term Testosterone Enanthate Use: Health Risks for American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0012) Testosterone Enanthate: A Promising Treatment for Osteoporosis in American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0013) Testosterone Enanthate: Medical Uses, Myths, and Performance Risks in American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Testosterone Enanthate's Impact on Male Fertility: Insights for American Men on TRT [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Testosterone Enanthate: A Promising Therapy for Chronic Pain in American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0016) Testosterone Enanthate: Medical Uses, Cultural Perceptions, and Ethical Concerns in the U.S. [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0017) Testosterone Enanthate: A Potential Aid in Stress Management for American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) Testosterone Enanthate: Enhancing Injury Recovery in American Males - Benefits and Risks [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0019) Testosterone Enanthate: Enhancing Immune Function in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0020) Testosterone Enanthate: Impacts on Hair Growth and Loss in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0021) Testosterone Enanthate: Enhancing Vitality in Aging American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) Ethical Dilemmas of Testosterone Enanthate Use in American Males: Medical vs. Enhancement [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) Optimizing Testosterone Enanthate Therapy: Dosage, Monitoring, and Lifestyle Integration [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Testosterone Enanthate's Impact on Appetite and Digestion in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Testosterone Enanthate: Enhancing Body Composition in American Males - Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Testosterone Enanthate's Impact on Vision and Eye Health in American Males: A Review [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0027) Testosterone Enanthate's Impact on Blood Sugar Levels in American Men: A Comprehensive Analysis [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0028) Testosterone Enanthate's Impact on Mental Clarity in American Males: Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0029) Testosterone Enanthate: Enhancing Endurance in American Male Athletes - Benefits and Risks [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Testosterone Enanthate: Benefits, Limitations, and Management for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Testosterone Enanthate Withdrawal: Symptoms, Management, and Long-Term Considerations [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Testosterone Enanthate: A Promising Therapy for Obesity in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Testosterone Enanthate: A Dual Approach to Treating Anemia in Hypogonadal Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0034) Testosterone Enanthate Therapy: Benefits and Risks for Men Over 50 [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0035) Testosterone Enanthate Boosts Skin Elasticity in American Males: Benefits and Risks [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0036) Testosterone Enanthate: Enhancing Mood in American Males with Low Testosterone [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Testosterone Enanthate's Impact on Joint Health in American Men: Benefits and Risks [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Testosterone Enanthate: Benefits, Risks, and Cost-Benefit Analysis for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0039) Testosterone Enanthate: A Vital Therapy for Muscle Wasting in American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0040) Testosterone Enanthate's Impact on Liver Health in American Men: Monitoring and Management [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Testosterone Enanthate: A Potential Treatment for Chronic Fatigue Syndrome in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Testosterone Enanthate's Role in Managing Diabetes Among American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0043) Testosterone Enanthate Therapy: Enhancing American Veterans' Health and Well-being [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0044) Testosterone Enanthate's Impact on Cardiovascular Endurance in American Men: Risks and Benefits [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0045) Testosterone Enanthate: A Novel Approach to Managing Allergies in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0046) Testosterone Enanthate: Enhancing Post-Surgical Recovery in American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0047) Testosterone Enanthate's Impact on Dental Health in American Males: A Comprehensive Review [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Testosterone Enanthate Therapy: Impacts on Life Expectancy and Quality of Life in Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) Testosterone Enanthate: A Promising Treatment for Autoimmune Disorders in American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0050) Testosterone Enanthate's Impact on Hearing Health in American Men: A Review [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0051) Testosterone Enanthate: Enhancing Respiratory Function in American Men [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0052) Testosterone Enanthate Therapy: Impacts on Kidney Function in American Males [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0053) Testosterone Enanthate: Emerging Treatment for Gastrointestinal Disorders in American Males [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0054) Testosterone Enanthate: Enhancing Neurological Health in American Men [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0055) Testosterone Enanthate: A New Approach to Managing Hypertension in American Males [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0056) Testosterone Enanthate: Benefits, Fertility Risks, and Hormonal Impact in American Males [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0057) Testosterone Enanthate's Role in Managing Respiratory Disorders in American Males [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0058) Testosterone Enanthate's Impact on Adrenal Health in American Males: A Comprehensive Analysis [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0059) Testosterone Enanthate's Impact on Immune Function in American Males: A Comprehensive Review [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0060) Testosterone Enanthate Therapy: Benefits, Risks, and Endocrine System Management [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0061) Testosterone Enanthate Therapy's Impact on Thyroid Function in American Men [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0062) Testosterone Enanthate: Emerging Dermatological Benefits for American Men [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0063) Testosterone Enanthate's Impact on Cardiovascular Health in American Males: A Review [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0064) Testosterone Enanthate: Enhancing Musculoskeletal Health in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0065) Testosterone Enanthate's Impact on Gastrointestinal Health in American Males [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0066) Testosterone Enanthate: Enhancing Hematological Health in American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0067) Testosterone Enanthate: Managing Metabolic Disorders in American Males [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0068) Testosterone Enanthate: Exploring Neurological Benefits in American Males [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0069) Testosterone Enanthate Boosts Immune Function in American Men: Research Insights [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0070) Testosterone Enanthate: Enhancing Gastrointestinal Health in American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) Testosterone Enanthate: Vital Role in Managing Hypogonadism and Endocrine Disorders [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Testosterone Enanthate's Metabolic Impact on American Males: Benefits and Risks [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0073) Testosterone Enanthate Therapy: Benefits, Risks, and Reproductive Health Impact [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0074) Testosterone Enanthate's Impact on Respiratory Health in American Males: A Review [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0075) Testosterone Enanthate Therapy: Cardiovascular Benefits and Risks in American Men [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0076) Testosterone Enanthate's Dermatological Effects on American Males: Acne, Hair Loss, and Skin Health [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0077) Testosterone Enanthate: A Promising Treatment for Musculoskeletal Disorders in American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0078) Testosterone Enanthate: A Promising Treatment for Hematological Disorders in American Men [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0079) Testosterone Enanthate: Treating Hypogonadism and Enhancing Men's Quality of Life [Last Updated On: April 21st, 2025] [Originally Added On: April 21st, 2025]
- 0080) Testosterone Enanthate: Benefits, Risks, and Management for American Males [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]