Video Link: https://vimeo.com/286243472
Video Download: Click Here To Download Video
Video Stream: Click Here To Stream Video
The Key Role This Hormone Plays in Regulating the Reproductive System
Luteinizing Hormone (LH) is produced by the pituitary gland and plays a vital role in controlling the reproductive system.
Luteinizing Hormone is a gonadotropic hormone (the hormone responsible for stimulating the gonads and monitoring reproductive activity) that is manufactured and secreted by cells  in the anterior pituitary gland.
in the anterior pituitary gland.
It plays a crucial role in regulating the function of the testes in men and ovaries in women.
In men, LH Leydig cells in the testicles promote both testosterone and sperm production.
Testosterone is also required for the development of masculine features such as strength, muscle size and strength, and the growth of facial hair.
Luteinizing Hormone performs different functions for women. LH plays different roles in the two parts of a woman's menstrual cycle.
For the first two weeks of the cycle, LH is necessary for stimulation of the ovarian follicles in the ovary that are responsible for the production of the female sex hormone oestradiol.
At the second part of the cycle, beginning around day 14, Luteinizing Hormone surges, which results in the ovarian follicle tearing and releasing a mature oocyte (egg) from the ovary.
This procedure is called ovulation, which is defined as the process where the egg travels down the fallopian tube where it can meet up with sperm, with the possible result being fertility (the ability to conceive children).
For the rest of the second cycle (weeks three and four), what is left of the ovarian follicle forms a corpus luteum, which is defined as a hormone-secreting structure that develops in an ovary after an ovum has been released but degrades after a few days unless pregnancy has begun.
If fertilization has come about, LH stimulates the corpus luteum to manufacture progesterone, a steroid hormone that preps the uterus for pregnancy.
In addition to the two cycles mentioned, there are also three phrases to the menstrual cycle:
- The Follicular phase. This is the first step of the cycle and starts on day one when bleeding begins, and the uterus lining starts to shed. When fertilization didn't occur in the last menstrual cycle, the uterus must shed the lining to prepare for the next cycle. This cycle's duration is usually three to five days, during which hormones must prepare the body for ovulation before the next phase begins.
- The Ovulation phase. In this second phase, estrogen levels multiply, flooding the uterus lining with blood and nutrients. These increased estrogen levels
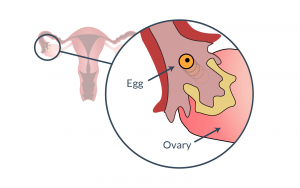 produce changes in cervical mucus, causing it to become slippery and thin. This makes a far easier path for sperm to find a waiting egg. This usually happens between seven and eleven days into the cycle.
produce changes in cervical mucus, causing it to become slippery and thin. This makes a far easier path for sperm to find a waiting egg. This usually happens between seven and eleven days into the cycle. - The pituitary gland also releases a flood of luteinizing hormone which bursts the follicle, pushing the ripened egg into the Fallopian tube. This signals the ripened egg to grow, mature, and smash through the follicle. The release of the egg = ovulation. The now free egg sails down the fallopian tube toward the womb. If fertilization does not occur soon, its survival time shrinks to around 24 hours.
- Sperm has a slightly longer lifespan and may arrive 24 hours later. Therefore, the time of maximum fertility is the day before and the day of ovulation. This is the ideal time for conception. The final step in the ovulation phase is progesterone release. Progesterone preps a fertilized egg by boosting the womb's lining with an increase in blood vessels.
- The Luteal phase. This starts with the formation of the corpus luteum and ends in either pregnancy or luteolysis (the structural and functional degradation of the corpus luteum (CL), which occurs at the end of the luteal phase of both the estrous and menstrual cycles in the absence of pregnancy). If the egg is fertilized, the body produces Human Chorionic Gonadotropin (hCG), a hormone produced by the embryo after implantation. This hormone keeps the follicle from shrinking and allows it to continue manufacturing estrogen and progesterone. This increased production keeps the uterus intact and keeps the fertilized egg (the pregnancy) going. If the egg is not fertilized within 24 hours, the corpus luteum dies and the levels of progesterone drop. The result of this is the uterine lining loses its extra blood supply, after about eleven to fourteen days, and your period (menstrual cycle) begins again.
The secretion of LH is initiated and controlled by the hypothalamic-pituitary-gonadal axis, a system that acts as a team. The hypothalamus releases Gonadotropin-releasing hormone, which attaches to receptors in the anterior pituitary gland which stimulates both the production and releasing of luteinizing hormone.
 This released LH is then carried into the blood stream where it binds to receptors in the testes and ovaries to regulate their hormone secretions and their production of sperm or eggs.
This released LH is then carried into the blood stream where it binds to receptors in the testes and ovaries to regulate their hormone secretions and their production of sperm or eggs.
The secretion of hormones from the gonads can inhibit the release of the gonadotropin-releasing hormone, and luteinizing hormone from the pituitary gland.
This results in a condition called negative feedback, defined as the levels of hormones released from the gonads falling and gonadotropin-releasing hormone and LH rising.
The importance of this occurring is that for men, testosterone controls this negative feedback. For women, estrogen and progesterone exercise the same effect except in the middle of the menstrual cycle.
When this happens, the high estrogen secretions from the ovary stimulate a flood of LH from the pituitary gland, resulting in ovulation.
Why the Level of Luteinizing Hormone is so Important
This balance of luteinizing hormone is the key to causing and maintaining fertility. As a result of this balance, substances that imitate the actions of gonadotropin-releasing hormone, luteinizing hormone, and follicle-stimulating hormone affect gonadal function in aided conception methods like in Vitro Fertilization (IVF).
Measuring the levels of LH in urine can predict the timing of the luteinizing hormone surge in women, and time ovulation. This ability to predict ovulation is vital for couples wishing to conceive.
Too high a level of LH can be an indicator of infertility. Polycystic ovary syndrome is a condition commonly associated with high levels of luteinizing hormone and lowered fertility. When this unfortunate condition is present, an imbalance between LH and follicle-stimulating hormone can cause an abnormal production of testosterone.
hormone and lowered fertility. When this unfortunate condition is present, an imbalance between LH and follicle-stimulating hormone can cause an abnormal production of testosterone.
Genetic conditions such as Klinefelter's syndrome (A male-only disorder and genetic condition in which a male is born with an extra copy of the X chromosome, resulting in small testicles and reduced sperm production) and Turner syndrome (A female chromosomal disorder in which a female is born with only one X chromosome, which inhibits ovarian function) can also cause high LH levels.
As mentioned earlier, LH levels are a delicate balance. Low levels also cause fertility problems. In men, low levels of Luteinizing hormone result in a condition called Kallman's syndrome (a genetic disease that delays puberty and causes infertility).
In women, ovulation does not occur when there are low levels of LH.
The Luteinizing Hormone Blood Test
The Luteinizing Hormone (LH) Blood Test is a measurement of the amount of LH in your bloodstream. There are several reasons for your health care provider to request an LH blood test. Here are a few of them…
- Difficulty in getting pregnant. LH levels of both women and men can affect fertility.
- Problems with menstrual periods. The amount of LH in your blood may help to determine the cause and best course of treatment.
- Delayed puberty. Again, LH levels may be the key to unraveling this mystery.
- Trouble with the pituitary gland.
- In a man, low testosterone levels.
- Determine if a woman has entered menopause.
 There are many possible causes of the problems listed above. Hopefully, the LH blood test will guide your physician on the right path to directly determine both the reasons for the symptoms and the correct treatment method.
There are many possible causes of the problems listed above. Hopefully, the LH blood test will guide your physician on the right path to directly determine both the reasons for the symptoms and the correct treatment method.
References
Luteinizing hormone and its dilemma in ovulation induction
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) New Research on Hormone Replacement Therapy [Last Updated On: January 21st, 2026] [Originally Added On: March 12th, 2021]
- 0002) LCN2 Hormone Suppresses Hunger and Stops Cravings! [Last Updated On: March 17th, 2026] [Originally Added On: April 7th, 2021]
- 0003) Melatonin: The Body's Master Clock [Last Updated On: January 16th, 2026] [Originally Added On: April 8th, 2021]
- 0004) Andropause From The Wikipedia Encyclopedia [Last Updated On: January 20th, 2026] [Originally Added On: April 12th, 2021]
- 0005) Finally Explained: The Mysterious Pineal Gland [Last Updated On: January 18th, 2026] [Originally Added On: April 30th, 2021]
- 0006) Hormone Therapy May Help Cut Alzheimer's Risk [Last Updated On: December 30th, 2025] [Originally Added On: May 18th, 2021]
- 0007) Androgel : Men Getting Their Mojo Back! [Last Updated On: May 12th, 2025] [Originally Added On: May 21st, 2021]
- 0008) HGH Secretagogue [Last Updated On: December 29th, 2025] [Originally Added On: May 22nd, 2021]
- 0009) Hormone Replacement Therapy Safe, Study Suggests [Last Updated On: May 17th, 2025] [Originally Added On: May 24th, 2021]
- 0010) The HGH Recommended Medical Dosage - The Importance of Blood Work [Last Updated On: December 28th, 2025] [Originally Added On: May 25th, 2021]
- 0011) Act Now to Prevent the Increasingly Common Condition of Hypothyroidism [Last Updated On: October 23rd, 2025] [Originally Added On: June 21st, 2021]
- 0012) A Toxic Hormone is Altering the Sex and Reproduction of Aquatic Life in United States Streams [Last Updated On: December 26th, 2025] [Originally Added On: August 16th, 2021]
- 0013) New Research: Cognitive Therapy Could Reduce Menopausal Hot Flashes [Last Updated On: December 25th, 2025] [Originally Added On: August 16th, 2021]
- 0014) Heart Benefits From Hormone Replacement Therapy? [Last Updated On: December 24th, 2025] [Originally Added On: August 18th, 2021]
- 0015) Risks of Hormones in Early Menopause Challenged [Last Updated On: December 23rd, 2025] [Originally Added On: August 24th, 2021]
- 0016) Comprehensive Hormone Replacement Therapy with Tesamorelin [Last Updated On: May 5th, 2025] [Originally Added On: September 18th, 2021]
- 0017) Early Hormone Replacement Therapy May Lower Alzheimer Risk [Last Updated On: December 16th, 2025] [Originally Added On: October 25th, 2021]
- 0018) Stimulate HGH: Growth Hormone Secretagogue: Sermorelin Acetate [Last Updated On: December 22nd, 2025] [Originally Added On: October 25th, 2021]
- 0019) Growth Hormone Therapy Reverses Biological Age In Groundbreaking Study [Last Updated On: December 13th, 2025] [Originally Added On: October 25th, 2021]
- 0020) Estrogen HRT May Reduce Breast Cancer Risk [Last Updated On: December 10th, 2025] [Originally Added On: October 26th, 2021]
- 0021) Hormone Replacement Therapy is Safe [Last Updated On: December 17th, 2025] [Originally Added On: October 26th, 2021]
- 0022) The Benefits of IGF-1 [Last Updated On: December 12th, 2025] [Originally Added On: October 26th, 2021]
- 0023) Insulin-Similar Growth Factor Benefits [Last Updated On: December 18th, 2025] [Originally Added On: October 26th, 2021]
- 0024) Growth Hormone Dosage [Last Updated On: December 9th, 2025] [Originally Added On: October 26th, 2021]
- 0025) Growth Hormone Sprays [Last Updated On: December 8th, 2025] [Originally Added On: October 26th, 2021]
- 0026) The Best Ways to Boost Growth Hormone [Last Updated On: December 15th, 2025] [Originally Added On: October 26th, 2021]
- 0027) Growth Hormone Explained [Last Updated On: December 19th, 2025] [Originally Added On: October 26th, 2021]
- 0028) What Men Need To Know About Testosterone And Growth Hormone [Last Updated On: December 6th, 2025] [Originally Added On: October 26th, 2021]
- 0029) Growth Hormone and Gene Therapy [Last Updated On: December 7th, 2025] [Originally Added On: October 26th, 2021]
- 0030) Growth Hormone and the Law [Last Updated On: December 5th, 2025] [Originally Added On: October 27th, 2021]
- 0031) Growth Hormone and the Hypothalamus Gland [Last Updated On: December 4th, 2025] [Originally Added On: October 27th, 2021]
- 0032) Growth Hormone and Testosterone Replacement Therapy [Last Updated On: January 28th, 2026] [Originally Added On: October 27th, 2021]
- 0033) Growth Hormone and Pneumonia [Last Updated On: December 3rd, 2025] [Originally Added On: October 27th, 2021]
- 0034) An Introduction to Growth Hormone [Last Updated On: December 2nd, 2025] [Originally Added On: October 27th, 2021]
- 0035) General Physician Versus Hormone Specialist – Some Symptoms Require a Specialist to Heal [Last Updated On: September 6th, 2025] [Originally Added On: March 18th, 2022]
- 0036) Hormone Impacts And Function Of HGH [Last Updated On: January 2nd, 2026] [Originally Added On: July 10th, 2022]
- 0037) Cheaping Out on HGH Therapy – JUST DON’T DO IT [Last Updated On: September 18th, 2025] [Originally Added On: July 12th, 2022]
- 0038) Slow Aging with Growth Hormone [Last Updated On: May 27th, 2025] [Originally Added On: July 17th, 2022]
- 0039) Hormone Therapies: How They Have Evolved and Are Evolving [Last Updated On: September 10th, 2025] [Originally Added On: February 10th, 2023]