Video Link: https://vimeo.com/291646852
Video Download: Click Here To Download Video
Video Stream: Click Here To Stream Video
Video Link: https://vimeo.com/291647020
Video Download: Click Here To Download Video
Video Stream: Click Here To Stream Video
Did you know?
Recent studies have confirmed the link between low testosterone (“Low-T”) and depression.
Did you know that clinical depression has been shown to have a direct relationship to low testosterone (“Low-T”)?
 Older men are at especially high risk for depression. Older men also usually experience a dramatic decline in their testosterone levels. Coincidence? Perhaps. But perhaps not.
Older men are at especially high risk for depression. Older men also usually experience a dramatic decline in their testosterone levels. Coincidence? Perhaps. But perhaps not.
But it is not only older men who are at risk for depression. Men of all ages who have Low-T are also more apt to be depressed.
Which Came First: the Chicken or the Egg?
The connection between low testosterone and depression is similar to the age-old question of “what came first; the chicken or the egg”?
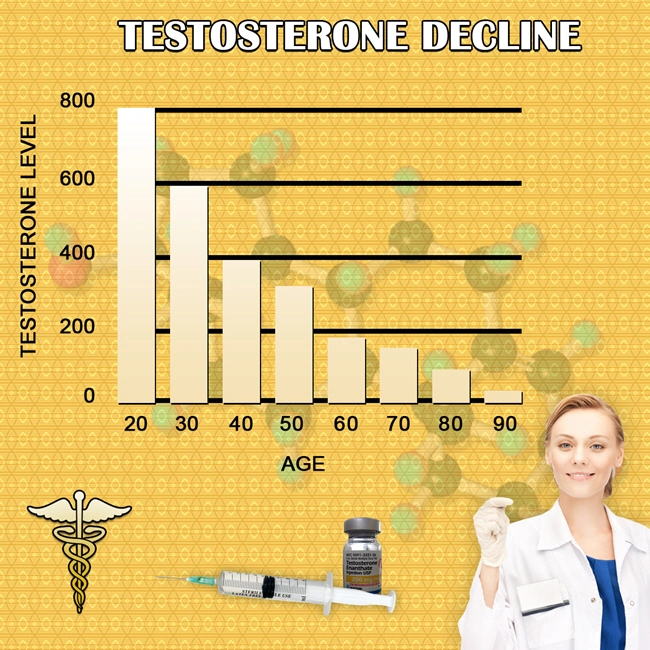
That is indeed a good question. To apply it to the Low-T and depression link, consider that testosterone levels begin a steady and inexorable decline in men starting at approximately age 30.
By the time men reach their mid-50s, approximately one-third of them suffer from Low-T.
Also, men who are overweight, diabetic, or have high blood pressure are far more prone to have unusually anemic testosterone levels.
Conversely, men who are battling the conditions mentioned above also often experience...you guessed it...Low-T.
So, does a lack of testosterone cause these afflictions? Or do these conditions cause testosterone to plummet?
Tough questions that are challenging to answer conclusively, since many of the symptoms of both conditions are nearly identical.
The research into this link has so far been inconclusive. There could be other factors at work that are precursors to these health problems. But currently, many signs point to a definitive relationship between Low-T and adverse health.
Add Depression to the List of Low-T Conditions
Depression has raised its ugly head and joined the Low-T hit parade. Just as men suffering from physical ailments are more likely to be diagnosed with low testosterone, so too are men who have depression more likely to have Low-T.
This link raises a depressing (pun intended) question. Do Low-T and all of the accompanying adverse health issues (muscle loss, joint aches and pains, fatigue, lethargy, hair loss where it’s needed and hair appearance where it’s NOT needed, brain fog, weight gain, fat accumulation, and lack of libido) cause depression?
Or does the depression that often accompanies aging and low testosterone levels result in a man losing his ability to fight the dreaded health deterioration that comes with aging...or even caring that his body is degenerating?
These questions are not easy to correctly and definitively answer. Like the earlier-mentioned physical symptoms of aging and depression, the conditions of Low-T and depression also have symptoms that overlap: memory problems, brain fog, anxiety, sadness, melancholy, and in appropriate anger.
One possibility obtained from a study of mice concluded that testosterone levels might influence serotonin amounts in the brain. Serotonin is a potent hormone that performs many essential functions. One of these functions is to stabilize and boost our moods.
As with so many other aspects, aging causes our serotonin levels to nose dive and inhibits older folks from absorbing what little serotonin they manufacture.
With these conflicting theories about the connection between Low-T and depression, it’s time to take a look at the research on the topic.
What the Research Says
A 2004 study aimed to clarify the link between the relationship of Low-T and depression. Another goal was to give guidance to medical professionals who have noticed the connection but are unsure as to how to proceed with treatment.
 Dr. Molly Shores lead the four-year study which consisted of 278 men over age 45. At the study’s conclusion, Dr. Shores and her team of researchers concluded that the men with Low-T were an incredible four times as likely to be diagnosed with clinical depression compared to men with standard testosterone ranges.
Dr. Molly Shores lead the four-year study which consisted of 278 men over age 45. At the study’s conclusion, Dr. Shores and her team of researchers concluded that the men with Low-T were an incredible four times as likely to be diagnosed with clinical depression compared to men with standard testosterone ranges.
In another study, 200 men who had been referred to an endocrinologist for testosterone deficiency demonstrated symptoms of depression. 56% of the study participants had been diagnosed with depression or were currently taking antidepressants, or showing severe symptoms of depression.
The study was led by Dr. Michael Irwig, MD, associate professor of medicine and director of the Center for Andrology at George Washington University, Washington. "Over half the men referred for borderline testosterone levels have depression," Irwig said at the annual meeting of The Endocrine Society.
Dr. Irwig also observed that the men were often overweight and were not fans of exercise, to put it mildly.
51% of the participants said that aside from walking they were mostly “couch potatoes” and performed no other activity. 27% of the men worked out one to three times a week, and 22% exercised at least four times a week.
Dr. Irwig stated that 39% of the participants were overweight and another 43% were obese. A mere 16% of the men were of standard weight, and a minuscule 2% were underweight.
An astonishing 89% of the study group revealed they had experienced erectile dysfunction (ED), 69% had diminished libido, 58% had fewer or no morning erections, 52% complained of fatigue, 42% suffered from insomnia, and 27% experienced brain fog and an inability to concentrate.
"A lot of these patients have all these co-morbidities and may be depression or undiagnosed depression," Irwig said. "For the patients who had undiagnosed depressive symptoms, I often recommend that they seek a formal evaluation from a mental health professional. For those who have been diagnosed and are overweight or obese, I do encourage weight loss and an exercise program using a pedometer. Loss of weight is associated with the body's ability to produce its own testosterone."
 Dr. Cynthia Stuenkel, MD, clinical professor of medicine at the University of California, San Diego, commented that "When a patient presents with some symptoms and is found to have a low testosterone level, as The Endocrine Society's guidelines recommend, we ask why this is. We know that some very clear endocrine reasons involve the hypothalamus, the pituitary, and the testicles that can be related to diseases that can cause low testosterone.”
Dr. Cynthia Stuenkel, MD, clinical professor of medicine at the University of California, San Diego, commented that "When a patient presents with some symptoms and is found to have a low testosterone level, as The Endocrine Society's guidelines recommend, we ask why this is. We know that some very clear endocrine reasons involve the hypothalamus, the pituitary, and the testicles that can be related to diseases that can cause low testosterone.”
She continued: "I always feel that the first step in treating these patients is to clarify what the diagnosis is because we might be able to fix it, we could remedy it. If there is not a clear diagnosis, then the next step we need to do is to repeat that testosterone test -- usually several times.”
She added that if the cause of Low-T is still not determined, the next step should be to delve into what is happening in the man’s life, his age, and other possible causes of his condition.
At that point, she said, it may be time to consider if "there is a role for a trial of testosterone therapy, again being mindful that there could be placebo effects."
Dr. Stuenkel concluded that the studies into this link are too few to be conclusive and said, "I think we need more studies to look into this."
Other Studies Have Shown Mixed Results
In recent years there has been a surge of double-blind, randomized, placebo-controlled trials on the depression-low testosterone link. The results have been inconclusive.
Sixteen trials that were analyzed concluded that testosterone is a useful treatment for depression in men. The trials looked at several different aspects to home in on regarding testosterone’s effectiveness:
Age. Testosterone was a more efficient mood-booster in men under age 60. In older men, testosterone was not as effective.
The degree of depression. Testosterone was most useful in men with either minor depression or dysthymia, a type of depression that has less intense symptoms but lasts longer. With severely depressed men, testosterone helped but not as much as with men with less severe depression.
Testosterone levels. Unsurprisingly, TRT was a mood elevator in men with low-T. But men with normal testosterone levels were not significantly helped.
A Japanese study observed 50 men with an average age of 57 who had low-T and were treated by urologists at the Kobe University Graduate School of Medicine in Japan.
At the start of the study 30 of the participants were diagnosed with depression. For this group, depression dropped after six months, and by the end of the survey, only 11 of the 30 were still afflicted with depression -- a significant drop.
A Chinese study produced similar, encouraging results. This study was conducted at the Department of Urology at Peking University People’s Hospital in Beijing, China. The group consisted of 160 men over age 50 who had low testosterone levels and had shown symptoms of low-T such as fatigue, sadness/grumpiness, physical decline, losing height, fewer erections, and deteriorating job performance.
Beijing, China. The group consisted of 160 men over age 50 who had low testosterone levels and had shown symptoms of low-T such as fatigue, sadness/grumpiness, physical decline, losing height, fewer erections, and deteriorating job performance.
During the six-month study, the men received either a placebo or oral testosterone undecanoate, 120-160 mg daily depending on their baseline testosterone levels. Initially, many of the men were stressed, experiencing erectile dysfunction, and reduced quality of life -- in short, the perfect definition of clinical depression.
However, after completing the treatment regimen, the men receiving TRT experienced vast improvements in all areas measured.
The subjects in the placebo group received no noticeable improvements in their depression.
Other studies have failed to unequivocally establish the Low-T/depression link, so the research continues.
The Mental Health Field Takes Notice
Mental health professionals are increasingly looking into the low testosterone link to depression to ensure that they do not overlook a possible treatment. This is especially true for patients who have not responded positively to antidepressants.
Low testosterone symptoms often are a cause of psychological problems such as:
Anxiety
Lowered ability to tolerate stress
Less assertiveness
More submissiveness
Irritability
Depression and lower mood
From looking at this list, it is obvious why psychiatrists are looking closely at testosterone replacement therapy.
The Limitations of Antidepressants
There is no question about it. For some people, antidepressants are a life-saver. Common selective serotonin reuptake inhibitors (SSRIs) like Prozac and Zoloft and norepinephrine-dopamine reuptake inhibitors (NDRI’s) like Wellbutrin have worked wonders and brought countless people back from the abyss of severe depression.
But these drugs don’t work for everyone. Some people have spent years and even decades on the prescriptions, as mentioned earlier, as well as Xanax and Ativan for anti-anxiety, Adderall for Attention Deficit Hyperactivity Disorder (ADHD), and other antidepressants like Remeron...all to no avail and no relief.
Worse, for some patients, these drugs cause horrendous side effects: digestive distress, nervousness, anxiety, dizziness, dry mouth, headache, and blurred vision.
 For these unfortunate folks, the severity of their depression is difficult for regular people to understand. Many people caught in the death-grip of depression have difficulty with basic life functions such as sleeping, working, or eating. In fact, some depression sufferers are challenged to even get out of bed in the morning.
For these unfortunate folks, the severity of their depression is difficult for regular people to understand. Many people caught in the death-grip of depression have difficulty with basic life functions such as sleeping, working, or eating. In fact, some depression sufferers are challenged to even get out of bed in the morning.
Their existence is feeling like they have waded into quicksand. They’re stuck and sinking fast.
So if standard treatments like the above-mentioned drugs do not provide relief, testosterone may be their last hope.
"We need to more completely understand the significance of the consequences of low testosterone, and to what extent testosterone therapy is effective in mitigating those consequences," said Dr. Christian Pike, a professor at USC's Leonard Davis School of Gerontology.
Dr. Pike feels that more research is required before testosterone replacement therapy (TRT) becomes a viable and safe treatment option for depression. But he added that "there is evidence from research in my lab and others suggesting that low testosterone increases the risks for Alzheimer's disease, metabolic syndrome, type 2 diabetes, and several other age-related conditions."
The Evidence Continues to Pour In
While not all studies on the link between low testosterone and depression agree, we continue to see more and more compelling evidence that points to low-T as a culprit in the crippling, cruel affliction called depression.
Increasing numbers of men in their 50s and 60s are suffering from both low testosterone and depression and are not passively accepting their gruesome fate. They are not willing to sit back and do nothing while their quality of life dwindles and falls off the cliff.
No, they are fighting back, “tooth and nail.” They are increasingly becoming aware of how testosterone fits into the depression equation...and they are taking action, massive action. And you can join them!
If you are experiencing extended periods of depression that exceed the usual ups-and-downs of everyday life, you owe it to yourself and the people who care about you to do something about it.
And that’s where our clinic is worth its weight in gold. We will run the lab tests, do the assessments, and discuss your treatment options in an easy to understand manner.
understand manner.
Our testosterone replacement therapy regimen is both safe and affordable. We will guide you every step of the way to let the light shine and pierce the dark veil of depression.
Don’t waste another day of your life in the death-clutch of this monster called depression. Get your life back!
This is not something you want to do on your own. We have the experience, equipment, and techniques to kick depression out of your life...once and for all!
References
Low Testosterone May Cause Depression
Can Testosterone Therapy Treat Depression In Men With Low T? A New Study Examines The Evidence
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) LabCorp Announces a Change to the Testosterone Reference Range [Last Updated On: April 16th, 2025] [Originally Added On: June 23rd, 2019]
- 0002) Important Facts About Testosterone Therapy Before Buying [Last Updated On: April 18th, 2025] [Originally Added On: July 13th, 2019]
- 0003) Soy: Does it Lower Testosterone? [Last Updated On: November 18th, 2025] [Originally Added On: August 30th, 2020]
- 0004) Testosterone Treatments May Successfully Reverse Type-2 Diabetes in Some Men [Last Updated On: April 15th, 2025] [Originally Added On: November 13th, 2020]
- 0005) Testosterone Replacement Therapy (TRT) May Prevent Heart Attacks and Diabetes [Last Updated On: April 21st, 2025] [Originally Added On: November 17th, 2020]
- 0006) New Study Finds Testosterone Does Not Increase Your Heart Attack Risk [Last Updated On: April 14th, 2025] [Originally Added On: January 11th, 2021]
- 0007) The Great Testosterone Debate [Last Updated On: April 20th, 2025] [Originally Added On: January 14th, 2021]
- 0008) Testosterone Replacement Therapy Lowers Heart Attack Risk [Last Updated On: April 19th, 2025] [Originally Added On: January 18th, 2021]
- 0009) New Study Says: The Benefits of Testosterone Replacement Therapy Outweigh The Risks [Last Updated On: April 22nd, 2025] [Originally Added On: January 19th, 2021]
- 0010) Male Menopause. Fact or Fiction ? [Last Updated On: April 23rd, 2025] [Originally Added On: January 20th, 2021]
- 0011) Testosterone: How Much Do You Really Know About This Masculine Hormone? [Last Updated On: November 6th, 2025] [Originally Added On: February 9th, 2021]
- 0012) Low-T: What are healthy levels of Testosterone and why is it difficult to measure? [Last Updated On: September 11th, 2025] [Originally Added On: April 3rd, 2021]
- 0013) Testosterone Therapy May Be Good for the Heart if You Have Low-T [Last Updated On: May 3rd, 2025] [Originally Added On: July 21st, 2021]
- 0014) A Recent Study Concludes: Testosterone DOES NOT Cause Prostate Cancer [Last Updated On: September 14th, 2025] [Originally Added On: August 16th, 2021]
- 0015) In the Battle Against Aging, When do the Risks Outweigh the Rewards? [Last Updated On: April 4th, 2025] [Originally Added On: August 18th, 2021]
- 0016) New Study Concludes: Boosting Testosterone Levels Lowers Men's Death Risk [Last Updated On: May 11th, 2025] [Originally Added On: August 20th, 2021]
- 0017) Testosterone Replacement Therapy Slows Prostate Cancer! [Last Updated On: April 2nd, 2025] [Originally Added On: September 13th, 2021]
- 0018) Research proves that Testosterone Therapy Boosts Fertility! [Last Updated On: April 5th, 2025] [Originally Added On: September 26th, 2021]
- 0019) Free Testosterone and Sex Hormone-Binding Globulin [Last Updated On: April 6th, 2025] [Originally Added On: October 15th, 2021]
- 0020) Testosterone Does Not Cause Heart Attacks [Last Updated On: April 7th, 2025] [Originally Added On: October 15th, 2021]
- 0021) Testosterone and Women [Last Updated On: April 8th, 2025] [Originally Added On: October 15th, 2021]
- 0022) Testosterone and Metabolic Syndrome [Last Updated On: April 3rd, 2025] [Originally Added On: October 15th, 2021]
- 0023) Testosterone and Disease Prevention [Last Updated On: March 31st, 2025] [Originally Added On: October 15th, 2021]
- 0024) Judge Vacates $140 Million Verdict in Testosterone Lawsuit [Last Updated On: April 1st, 2025] [Originally Added On: October 15th, 2021]
- 0025) Testosterone and Estrogen [Last Updated On: April 9th, 2025] [Originally Added On: October 16th, 2021]
- 0026) Testosterone and Aging [Last Updated On: April 10th, 2025] [Originally Added On: October 16th, 2021]
- 0027) Testosterone Replacement Therapy (TRT) Benefits [Last Updated On: April 11th, 2025] [Originally Added On: October 16th, 2021]
- 0028) Testosterone and Male Menopause [Last Updated On: March 30th, 2025] [Originally Added On: October 16th, 2021]
- 0029) Testosterone Battles Obesity [Last Updated On: March 29th, 2025] [Originally Added On: October 16th, 2021]
- 0030) Why You Need Testosterone Replacement Therapy [Last Updated On: May 14th, 2025] [Originally Added On: October 16th, 2021]
- 0031) Testosterone FAQ's [Last Updated On: May 13th, 2025] [Originally Added On: October 25th, 2021]
- 0032) How Testosterone Impacts Sexual Preferences In Men and Women [Last Updated On: March 28th, 2025] [Originally Added On: October 30th, 2021]
- 0033) Growth Hormone and The Thyroid Gland [Last Updated On: April 24th, 2025] [Originally Added On: November 19th, 2021]
- 0034) How Does Masturbation Affect Testosterone Levels? Exploring the Science [Last Updated On: May 24th, 2025] [Originally Added On: March 27th, 2022]
- 0035) Testosterone Therapy Increasingly Used to Help Men Take Control of Aging [Last Updated On: May 25th, 2025] [Originally Added On: May 30th, 2022]
- 0036) The many benefits of Testosterone Replacement Therapy (TRT) [Last Updated On: November 1st, 2025] [Originally Added On: June 13th, 2022]
- 0037) Tlando Testosterone - A Brand New Way to Treat Low-T Safely with a Testosterone Pill [Last Updated On: May 28th, 2025] [Originally Added On: July 12th, 2022]
- 0038) Safe Tlando Testosterone Changes Landscape of Low-T Therapy [Last Updated On: May 30th, 2025] [Originally Added On: August 15th, 2022]
- 0039) Systems to Monitor Testosterone Replacement Therapy (TRT) [Last Updated On: October 12th, 2025] [Originally Added On: September 21st, 2022]
- 0040) Testosterone May Help You Keep Your Job (Or Find Another) [Last Updated On: June 12th, 2025] [Originally Added On: October 4th, 2022]
- 0041) Toxic Chemicals are Killing your testosterone…And your Manhood! [Last Updated On: November 28th, 2025] [Originally Added On: October 10th, 2022]
- 0042) A new study reveals that Testosterone improves body composition in men with low testosterone! [Last Updated On: October 22nd, 2025] [Originally Added On: October 17th, 2022]
- 0043) A former Mr. Olympia speaks about testosterone [Last Updated On: October 10th, 2025] [Originally Added On: November 8th, 2022]
- 0044) Testosterone Blockers Thwart Melanoma [Last Updated On: June 9th, 2025] [Originally Added On: December 11th, 2022]