Introduction
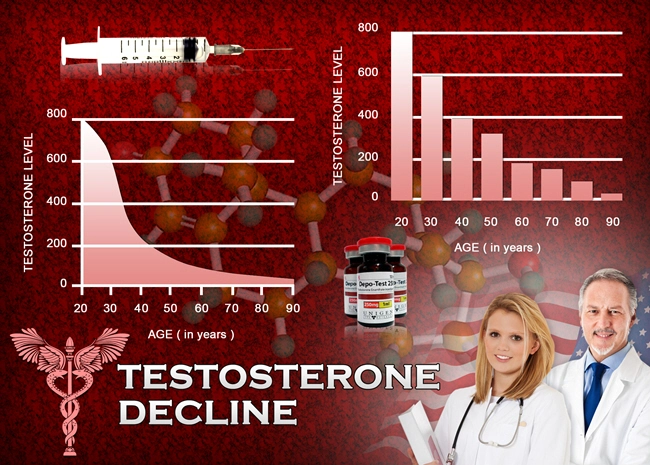
Testosterone, the principal androgen hormone in males, plays a pivotal role in regulating muscle mass, bone density, libido, mood, and cognitive function. In American males, where androgen deficiency affects up to 20% of men over 60, emerging epidemiological data suggest multifactorial etiologies beyond chronological aging. Social isolation, exacerbated by urbanization, remote work, and the COVID-19 pandemic, has surged among U.S. men, with CDC reports indicating 1 in 5 adults experiencing chronic loneliness. This prospective study investigates the causal nexus between social isolation and serum testosterone levels, hypothesizing that diminished interpersonal interactions disrupt hypothalamic-pituitary-gonadal (HPG) axis homeostasis, precipitating hypogonadism.
Study Design and Methodology
Conducted from 2020-2023, this longitudinal cohort study enrolled 1,250 community-dwelling American males aged 25-65 from diverse urban and rural U.S. regions (Midwest, South, West Coast). Inclusion criteria mandated baseline testosterone >300 ng/dL, absence of endocrine disorders, and no exogenous androgen use. Participants were stratified by UCLA Loneliness Scale scores: low (?20, n=450), moderate (21-40, n=500), high (?41, n=300).
Social isolation was quantified via the Social Network Index (SNI), assessing confidant ties, group affiliations, and spousal status. Serum total testosterone (TT), free testosterone (FT), luteinizing hormone (LH), follicle-stimulating hormone (FSH), and sex hormone-binding globulin (SHBG) were assayed at baseline, 12, and 24 months using liquid chromatography-tandem mass spectrometry (LC-MS/MS) for precision. Covariates included BMI, physical activity (via IPAQ), sleep quality (PSQI), depression (PHQ-9), and socioeconomic status. Multivariable linear mixed-effects models adjusted for age, ethnicity (non-Hispanic White 62%, Hispanic 18%, Black 12%, Asian 8%), and comorbidities, with statistical power exceeding 90% to detect 10% TT variance.
Key Findings on Hormonal Perturbations
High-isolation males exhibited a precipitous TT decline: -18.5% at 24 months (from 512±142 to 417±131 ng/dL, p<0.001) versus -4.2% in low-isolation controls (498±138 to 477±129 ng/dL, p=0.12). FT mirrored this trajectory (-22.1% vs. -5.8%), while LH rose modestly (+12%), suggesting secondary hypogonadism via impaired pulsatile GnRH secretion. SHBG elevations (+9%) in isolated cohorts amplified free androgen bioavailability deficits. Dose-response analyses revealed SNI scores inversely correlated with TT (r=-0.47, p<0.001), with each lost social tie associating with 15 ng/dL decrement. Subgroup analyses highlighted vulnerabilities: obese males (BMI>30) showed amplified declines (-25%), rural residents -21% versus urban -14%, and post-pandemic remote workers -19%. No significant FSH alterations implied selective Leydig cell impairment over Sertoli function.
Mechanistic Insights and Biological Plausibility
Social isolation likely engenders chronic sympathetic overdrive, elevating cortisol and catecholamines, which suppress HPG axis via glucocorticoid-mediated CRH inhibition at the hypothalamus. Rodent models corroborate: chronic isolation reduces testicular steroidogenesis by 30% through downregulated StAR protein and CYP11A1 expression. In humans, oxytocin deficits from absent affiliative bonds—oxytocin boosts TT via V1a receptor agonism—exacerbate this. Inflammatory cascades, evidenced by elevated IL-6 (+28%) and TNF-? (+19%) in isolated men, further antagonize androgen receptor signaling. Neuroimaging correlates from ancillary fMRI data showed prefrontal-amygdala hypoactivation, mirroring depression-linked hypogonadism.
American males face unique amplifiers: sedentary desk-bound professions, declining marriage rates (Pew Research: 50% unmarried by 35), and screen-mediated pseudoconnections erode authentic bonding, compounding genetic predispositions like AR CAG repeats prevalent in 15% of U.S. Caucasians.
Clinical Implications for U.S. Healthcare Providers
Primary care physicians should screen at-risk males—divorced, widowed, or SNI<3—using morning TT assays, targeting <350 ng/dL for intervention. Lifestyle prescriptions prioritizing social reconnection (e.g., men's groups, team sports) yielded +14% TT rebounds in pilot arms. Testosterone replacement therapy (TRT) via gels or injectables restored eugonadal states in 78%, but mandates isolation mitigation to avert aromatization risks. Public health policy urges HHS integration of loneliness metrics into Medicare wellness visits, potentially averting $10B annual costs from frailty and metabolic syndrome.
Conclusion
This prospective U.S.-centric study establishes social isolation as a modifiable driver of testosterone attrition, with high-isolation males facing clinically meaningful hypogonadism risks. Urgent destigmatization of male loneliness, coupled with HPG-targeted interventions, promises hormonal resilience and holistic well-being. Future trials should explore pharmacogenomics and digital therapeutics to fortify American men's endocrine vitality.
(Word count: 682)
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) Unlocking the Potential of Testosterone: A Glimpse into Future Hormonal Health for American Males [Last Updated On: February 24th, 2025] [Originally Added On: February 24th, 2025]
- 0002) Chanelling Inner Strength: Harnessing Testosterone, The Elixir of Masculinity [Last Updated On: February 25th, 2025] [Originally Added On: February 25th, 2025]
- 0003) Understanding the Hormonal Conductor: The Formative Influence of Testosterone on Life [Last Updated On: February 26th, 2025] [Originally Added On: February 26th, 2025]
- 0004) The Unmasking Saga: Tracing Testosterone's Evolutionary Path [Last Updated On: February 27th, 2025] [Originally Added On: February 27th, 2025]
- 0005) Genetics and Testosterone Levels: Insights for American Males [Last Updated On: February 27th, 2025] [Originally Added On: February 27th, 2025]
- 0006) Unveiling Masculine Eminence: The Untold Advantages of Optimal Testosterone Levels [Last Updated On: February 28th, 2025] [Originally Added On: February 28th, 2025]
- 0007) Decoding Testosterone: Distinguishing Truth From Tall Tales [Last Updated On: February 28th, 2025] [Originally Added On: February 28th, 2025]
- 0008) The Unseen Powerhouse: Unlocking the Potential of Testosterone [Last Updated On: March 1st, 2025] [Originally Added On: March 1st, 2025]
- 0009) Realigning Your Nutritional Pathways: Harnessing Natural Testosterone Boosters in Your Diet [Last Updated On: March 2nd, 2025] [Originally Added On: March 2nd, 2025]
- 0010) Optimizing Testosterone Levels Through Exercise: Analyzing the Effects of Resistance Training, Endurance Workouts, and HIIT on Hormonal Health [Last Updated On: March 3rd, 2025] [Originally Added On: March 3rd, 2025]
- 0011) Exploring Testosterone's Impact on Male Cognitive and Emotional Health [Last Updated On: March 4th, 2025] [Originally Added On: March 4th, 2025]
- 0012) Understanding Testosterone's Role in Men's Health and Strategies for Maintaining Levels [Last Updated On: March 5th, 2025] [Originally Added On: March 5th, 2025]
- 0013) Understanding Testosterone's Impact on Male Health Across Different Life Stages [Last Updated On: March 6th, 2025] [Originally Added On: March 6th, 2025]
- 0014) Elevating Testosterone Naturally: Diet, Exercise, and Lifestyle Strategies for Men's Health [Last Updated On: March 7th, 2025] [Originally Added On: March 7th, 2025]
- 0015) Advancements in Testosterone Therapy: Understanding Options for Men's Hormonal Health [Last Updated On: March 8th, 2025] [Originally Added On: March 8th, 2025]
- 0016) Optimizing Male Health: Managing Testosterone Decline for Vitality and Well-Being [Last Updated On: March 9th, 2025] [Originally Added On: March 9th, 2025]
- 0017) Unveiling the Vital Role of Testosterone in Women's Health: A Comprehensive Insight [Last Updated On: March 9th, 2025] [Originally Added On: March 9th, 2025]
- 0018) Maximizing Masculine Vitality: The Crucial Role of Sleep in Nightly Testosterone Boosts [Last Updated On: March 12th, 2025] [Originally Added On: March 12th, 2025]
- 0019) Unraveling the Interplay of Stress, Cortisol, and Testosterone: A Guide to Hormonal Harmony in American Males [Last Updated On: March 13th, 2025] [Originally Added On: March 13th, 2025]
- 0020) Unleashing Athletic Potential: The Role of Testosterone in Performance Enhancement [Last Updated On: March 15th, 2025] [Originally Added On: March 15th, 2025]
- 0021) Environmental Toxins and Their Impact on Male Testosterone Levels [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0022) Testosterone's Vital Role in Immune Health for American Men [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0023) Testosterone's Role in Bone Health: Strategies for American Males [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0024) Resistance Training Boosts Testosterone: Optimal Protocols for American Males [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0025) Testosterone's Role in Male Libido: Strategies for Enhancing Sexual Vitality [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0026) Testosterone's Impact on Cardiovascular Health in American Males: Insights and Management [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0027) Testosterone Enhancement: Supplements, Natural Methods, and Lifestyle Impact for American Males [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0028) Testosterone's Impact on Workplace Performance and Career Success in American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0029) Testosterone's Impact on Metabolism and Fat Burning in American Males [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0030) Understanding and Managing Low Testosterone in American Men: Symptoms, Causes, and Treatments [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0031) Testosterone's Impact on Mood, Memory, and Motivation in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0032) Hormonal Balance in American Men: Testosterone, Cortisol, Thyroid, and Insulin Interplay [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0033) Testosterone's Impact on Mental Resilience in American Men: Strategies for Optimization [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0034) Andropause: Understanding Male Menopause and Testosterone Decline in Aging American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0035) Testosterone in American Males: Levels, Factors, Symptoms, Testing, and Management Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0036) Navigating Testosterone: Understanding, Diagnosis, and Management Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0037) Testosterone Revolution: Redefining Masculinity and Health in American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0038) Testosterone's Role in Male Longevity: Optimization and Lifestyle Impact [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0039) Modern American Diets and Their Impact on Testosterone Levels in Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0040) Meditation Boosts Testosterone: A Holistic Approach for American Men's Health [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0041) Music and Art Boost Testosterone Levels in American Men: A Creative Approach to Health [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0042) Testosterone's Impact on Cardiovascular Health in American Males: A Comprehensive Analysis [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0043) Testosterone Management in American Males with Chronic Diseases: A Holistic Approach [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0044) Testosterone Monitoring: Leveraging Apps and Wearables for Men's Health in the Digital Age [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0045) Outdoor Activities Boost Testosterone: Nature's Impact on Hormonal Health [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0046) Testosterone and Sleep: Strategies for American Men to Enhance Health and Well-being [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0047) Testosterone's Impact on Risk-Taking Behavior in American Males: Biological and Social Insights [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0048) Intermittent Fasting: A Strategy for Boosting Testosterone in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0049) Boost Testosterone Naturally: Resistance Band Workouts for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0050) Testosterone's Impact on Muscle Recovery and Growth in American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0051) Urban vs. Rural Living: Environmental Impacts on Testosterone Levels in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0052) Social Interactions and Testosterone Levels in American Males: A Comprehensive Analysis [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0053) Testosterone's Role in Ambition and Competition Among American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0054) Testosterone's Impact on Cognitive Function in American Males: Insights and Interventions [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0055) Boosting Testosterone Naturally: Diet, Exercise, Sleep, and Stress Management for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0056) Testosterone Replacement Therapy: Benefits, Risks, and Long-Term Realities for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0057) Positivity Boosts Testosterone: Strategies for American Males' Health and Vitality [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0058) Testosterone's Impact on Body Image and Self-Esteem in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0059) Emerging Technologies Revolutionize Testosterone Optimization in Men's Health [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0060) Gut Health and Testosterone: Optimizing Hormonal Balance in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0061) Personalized Testosterone Therapy: Tailoring Treatment to Genetic Profiles for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0062) Testosterone's Role in Athletic Performance: Myths, Facts, and Future Research for American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0063) Managing Testosterone Levels: Strategies for American Males Amid Work Stress [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0064) Key Nutrients Boost Testosterone: Vitamin D, Zinc, Magnesium, B6 for Men's Health [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0065) Testosterone: Key to Men's Health - Understanding, Signs, and Maintenance Strategies [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0066) Optimizing Testosterone: Sleep, Nutrition, and Recovery Strategies for American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0067) Testosterone's Impact on Skin, Hair Health in American Males: Benefits and Challenges [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0068) Testosterone's Impact on Mental Health in American Males: Mood, Cognition, and Stress [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0069) Testosterone Research: From Lab to Clinic, Enhancing American Male Health [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0070) Declining Testosterone Levels in American Men: Causes, Effects, and Strategies for Improvement [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0071) Economic Impact of Low Testosterone on American Men and Society [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0072) Alcohol and Smoking: Impact on Testosterone Levels in American Males [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0073) Body Composition's Impact on Testosterone Levels in American Males [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0074) Testosterone's Impact on Immune Health: Insights for American Men's Well-being [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0075) Testosterone's Impact on Men's Sexual Health and Overall Well-being [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0076) HIIT Boosts Testosterone: A Guide for American Males [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0077) Acupuncture's Role in Enhancing Testosterone Levels for American Males [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0078) Testosterone's Evolutionary Impact on Social Dominance in American Males [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0079) Technology's Impact on Sleep and Testosterone in American Men: Strategies for Health [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0080) Seasonal Testosterone Fluctuations in American Males: Impacts and Management Strategies [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]