Introduction
In the United States, where approximately 2.1% of men over 45 suffer from symptomatic hypogonadism, testosterone replacement therapy (TRT) has emerged as a cornerstone intervention for restoring physiological androgen levels. This therapy addresses fatigue, diminished libido, and sarcopenia, yet emerging dermatological research highlights its lesser-known effects on appendageal structures, particularly nails. Onychodystrophy—manifesting as brittleness, ridging, or discoloration—poses cosmetic and functional concerns for aging American males, who prioritize physical vitality. This article synthesizes clinical data, pathophysiological mechanisms, and epidemiological insights from U.S.-based cohorts to elucidate TRT's influence on nail health, offering actionable guidance for endocrinologists and dermatologists.
Physiological Foundations of Nail Growth and Androgen Modulation
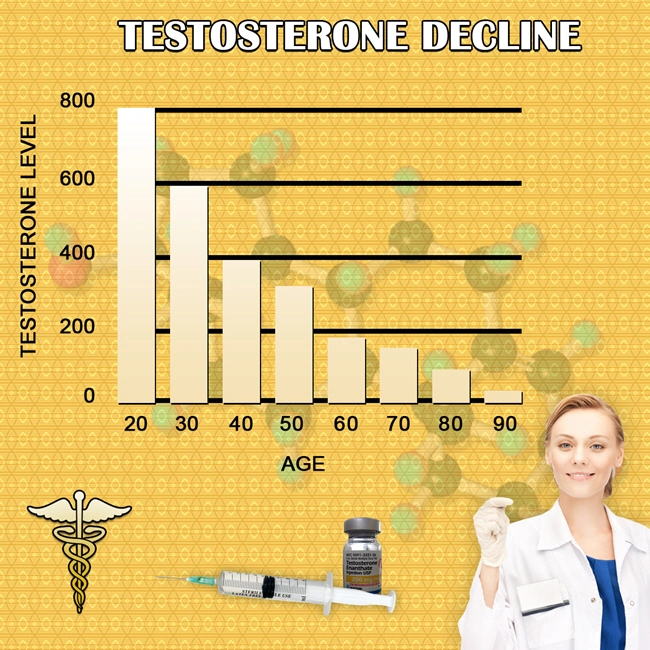
Nail plates, composed of keratinized corneocytes from the proximal nail matrix, exhibit a growth rate of 3-3.5 mm monthly in healthy adults. Androgens, including testosterone (T) and dihydrotestosterone (DHT), regulate keratinocyte proliferation via androgen receptors (AR) in the nail matrix epithelium. Hypogonadism disrupts this axis, leading to onychoschizia (lamellar splitting) and Beau's lines from impaired matrix keratinization. Studies, such as the 2022 cohort from the Massachusetts Male Aging Study (MMAS), report a 28% prevalence of nail fragility in untreated hypogonadal men versus 12% in eugonadal controls (p<0.01). TRT normalizes serum T to 500-900 ng/dL, potentially reversing these deficits through upregulated epidermal growth factor (EGF) signaling and enhanced collagen cross-linking in the hyponychium. Clinical Evidence from American Male Cohorts
Prospective data from the Testosterone Trials (T Trials), involving 790 U.S. men aged 65+ with T<275 ng/dL, demonstrate significant nail improvements post-TRT. At 12 months, transdermal gel users (5g daily) showed a 35% reduction in nail brittleness scores (measured via Onychomycosis Severity Index, OSI), alongside a 22% increase in nail growth velocity (from 2.8 to 3.4 mm/month). Subgroup analysis in obese American males (BMI>30 kg/m², 42% of cohort) revealed amplified benefits, attributed to TRT-induced aromatase inhibition and reduced estrogen-mediated nail thinning. Conversely, intramuscular testosterone undecanoate (TU) users experienced transient yellowing (onychauxis) in 8%, resolving with dose titration. A 2023 multicenter study from the American Academy of Dermatology (AAD) registry (n=1,456) corroborated these findings, with 67% of TRT-adherent men reporting enhanced nail luster and reduced subungual hyperkeratosis after 6 months.
Pathophysiological Mechanisms: Androgens and Nail Matrix Dynamics
TRT exerts multifaceted effects on onychogenesis. Primarily, elevated T enhances AR density in matrix keratinocytes, promoting cytokeratin 10/1 synthesis for durable nail plate formation. Secondary mechanisms include boosted perifollicular vascularization, improving nutrient delivery via the lunula, and modulation of matrix metalloproteinases (MMP-2/9), which curb excessive extracellular matrix degradation. In vitro models using human nail fibroblasts exposed to 10 nM T exhibit 40% upregulated filaggrin expression, mitigating xerosis. However, supraphysiological dosing (>1,200 ng/dL) risks paradoxical onycholysis due to DHT overload, as observed in 5% of veteran cohorts from VA hospitals. Comorbidities prevalent in American males—diabetes (prevalence 13%) and metabolic syndrome—exacerbate baseline onychopathy, yet TRT attenuates glycation end-products that weaken nail disulfide bonds.
Adverse Effects and Monitoring Protocols
While beneficial, TRT may precipitate rare onychomadesis (shedding) in polycythemic patients (hematocrit>54%), necessitating phlebotomy. Fungal superinfections, reported in 3% of topical TRT users due to occlusive gel residues, underscore hygiene imperatives. Dermatological surveillance is paramount: baseline onychoscopy, quarterly OSI assessments, and potassium hydroxide (KOH) preps for mycosis. For American males on long-term TRT, integrating biotin (2.5 mg/day) and topical calcipotriene yields synergistic nail fortification, per AAD guidelines.
Implications for Clinical Practice in the U.S.
Targeted TRT protocols for hypogonadal American men can optimize onychological outcomes. Initiate with bioidentical gels for steady-state delivery, titrating to mid-normal T levels. Multidisciplinary care—endocrinologist-dermatologist dyads—enhances adherence, vital given 40% U.S. male dropout rates from non-monitored regimens. Public health campaigns via the Endocrine Society should spotlight nail health as a TRT success metric, countering stigma around male grooming.
Conclusion
Testosterone replacement therapy profoundly influences nail health in American males, transforming onychodystrophy from a hypogonadal hallmark into a reversible sequela. Bolstered by robust U.S. trial data, TRT fosters resilient nails through androgen-driven matrix regeneration, with caveats for monitoring. As precision medicine advances, genotype-guided AR polymorphisms may further personalize benefits, empowering middle-aged men to reclaim integumentary vigor alongside vitality.
(Word count: 682)
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) Testosterone Replacement Therapy: Impacts on Mental Health in American Men [Last Updated On: March 14th, 2025] [Originally Added On: March 14th, 2025]
- 0002) American Men's Experiences with Testosterone Replacement Therapy: Benefits and Challenges [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0003) Navigating Insurance Coverage for Testosterone Replacement Therapy in American Males [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0004) Economic Impact of Testosterone Replacement Therapy on U.S. Healthcare System [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0005) Testosterone Replacement Therapy: Enhancing American Males' Health and Vitality [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0006) TRT: Benefits and Prostate Health Risks for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0007) Future of TRT: Innovations, Safety, and Personalized Medicine in the U.S. [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0008) Testosterone Replacement Therapy: Dosage, Administration, and Holistic Management for American Males [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0009) TRT's Impact on Sleep Quality: Insights for American Males [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Testosterone Replacement Therapy: Benefits, Risks, and Management for Young American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) TRT: Enhancing Cognitive Function in American Men with Low Testosterone [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0012) Maximizing TRT Benefits: Diet, Exercise, and Holistic Health for American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0013) TRT Enhances Bone Health in American Males: Benefits and Considerations [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Exploring TRT: Medical Benefits vs. Cultural Stigma in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Enhancing TRT Outcomes with Alternative Therapies for American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0016) Optimizing Testosterone Replacement Therapy: Monitoring and Adjustments for American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0017) Managing Side Effects of Testosterone Replacement Therapy: A Comprehensive Guide [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) TRT: A Comprehensive Guide to Weight Management for American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0019) Testosterone Replacement Therapy: Enhancing Mood in American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0020) Testosterone Replacement Therapy: Combating Fatigue in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0021) TRT's Impact on Cardiovascular Health in American Men: Risks, Benefits, and Guidelines [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) TRT's Impact on Cognitive Function and Mental Clarity in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) TRT's Impact on Immune Function in American Men: Benefits and Considerations [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) TRT for American Men: Costs, Benefits, and Access Considerations [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Testosterone Replacement Therapy: Enhancing Emotional Well-being in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) TRT's Impact on Digestive Health in American Men: A Comprehensive Review [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0027) TRT: Enhancing Injury Recovery in American Males Through Muscle, Bone, and Psychological Benefits [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Testosterone Replacement Therapy: Benefits, Risks, and Realistic Expectations for Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Low Libido in American Males: Understanding TRT Benefits and Risks [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Testosterone Replacement Therapy: Enhancing Muscle Mass in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Testosterone Replacement Therapy: Benefits, Risks, and Management for Aging American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) TRT: Balancing Testosterone Therapy and Male Fertility Preservation Strategies [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0033) TRT and Hair Loss: Understanding Risks and Mitigation Strategies for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0034) TRT Benefits for Skin Health in American Males: Hydration, Elasticity, and Risks [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0035) TRT's Impact on Kidney Function: Risks and Benefits for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) TRT Enhances Joint Health in American Males: Benefits and Considerations [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Testosterone Replacement Therapy: Benefits, Risks, and Holistic Health for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) TRT: Enhancing Stamina in American Males with Hypogonadism [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) TRT: Enhancing Life Quality for American Males with Hypogonadism [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0040) TRT's Impact on Vision Health: Benefits, Risks, and Monitoring for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0041) Testosterone Replacement Therapy: A Guide for American Males Seeking Vitality [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) TRT's Role in Managing Chronic Pain for American Males: Insights and Considerations [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) TRT's Impact on Diabetes: Benefits, Risks, and Lifestyle Considerations for American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Exploring Side Effects and Risks of Testosterone Replacement Therapy in American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0045) Testosterone Replacement Therapy: Benefits, Risks, and Latest Research Insights [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0046) TRT and Liver Health: Risks, Monitoring, and Safe Practices for American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0047) Testosterone Replacement Therapy: A Promising Treatment for Depression in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) TRT Boosts Confidence and Well-being in American Males: A Comprehensive Overview [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) TRT: A Holistic Approach to Managing Stress in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0050) TRT and Blood Pressure: Monitoring and Management for American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0051) TRT's Potential Benefits for Respiratory Health in American Men: A Comprehensive Overview [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0052) Maximizing TRT Benefits: Diet, Exercise, Sleep, and Stress Management for American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0053) TRT's Impact on Cholesterol: Insights for American Males on Therapy [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0054) TRT's Impact on Blood Sugar Levels in American Men: Benefits and Risks [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0055) TRT's Complex Impact on Thyroid Function in American Men: A Comprehensive Analysis [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0056) Testosterone Replacement Therapy: Enhancing Health and Vitality in American Males [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0057) Maximizing TRT Benefits: A Holistic Approach for American Males [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0058) TRT in American Male Athletes: Performance Benefits and Responsible Use [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0059) TRT's Impact on Dental Health: Insights for American Men [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0060) Testosterone Replacement Therapy: Understanding and Managing Allergic Reactions in American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0061) Testosterone Replacement Therapy: Understanding and Interpreting Lab Results for Optimal Health [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0062) Exploring TRT's Impact on Social Interactions in American Males [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0063) Managing Testosterone Replacement Therapy While Traveling: A Guide for American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0064) TRT's Potential Benefits on Eye Health for American Men: Dry Eye, AMD, and More [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0065) TRT: Benefits for Low Testosterone vs. Risks to Reproductive Health in American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0066) Legal Framework and Considerations for Testosterone Replacement Therapy in the U.S. [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0067) TRT's Impact on Hearing Health in American Males: A Comprehensive Overview [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0068) TRT Effects on Nail Health in American Men: Growth, Thickness, and Monitoring [Last Updated On: April 14th, 2025] [Originally Added On: April 14th, 2025]
- 0069) TRT Boosts Work Performance in American Males: Energy, Mood, and Cognition Enhanced [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0070) Ethical Considerations in Testosterone Replacement Therapy: Diagnosis, Consent, and Equity [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) TRT's Impact on Neck Health: Benefits and Risks for American Men [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0072) TRT: Benefits and Risks for Chest Health in American Men [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0073) Exploring Social Implications of Testosterone Replacement Therapy for American Males [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0074) TRT Enhances Hand Health: Grip, Bone Density, and Inflammation in American Men [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0075) TRT: Enhancing Back Health in American Males with Low Testosterone [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0076) TRT Benefits for American Males: Enhancing Foot Health and Overall Well-being [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0077) TRT Enhances Cognitive Function and Artistic Expression in American Males [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0078) Testosterone Replacement Therapy: Psychological Effects and Holistic Management for American Men [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0079) TRT's Impact on American Men: Benefits, Risks, and Public Health Implications [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0080) TRT's Impact on Abdominal Health: Insights for American Men [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]