Introduction
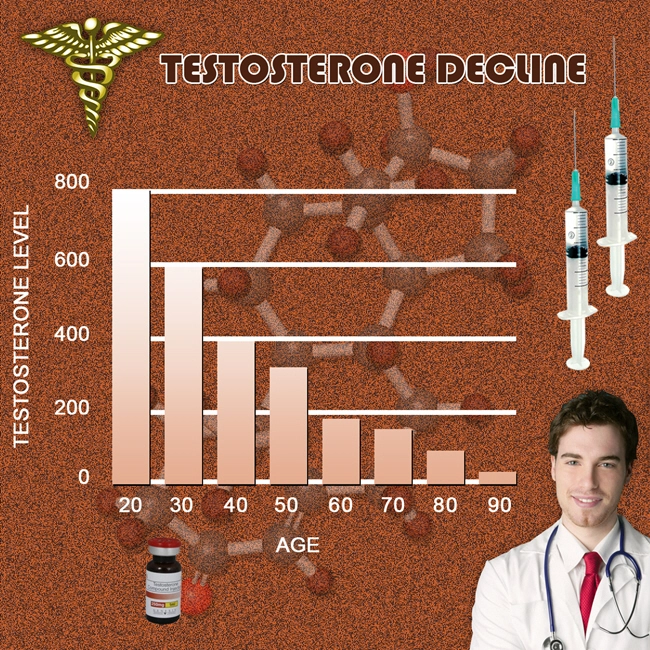
Allergic rhinitis, commonly known as hay fever, affects over 60 million Americans annually, with a notable prevalence among males aged 20-64, where environmental allergens exacerbate symptoms like nasal congestion, sneezing, and pruritus. In the United States, hypogonadism—characterized by deficient testosterone production—affects approximately 4-5 million men, correlating with dysregulated immune responses. Pfizer's Depo-Testosterone (testosterone cypionate injectable suspension) has emerged as a cornerstone of testosterone replacement therapy (TRT), traditionally prescribed for hypogonadism. Emerging immunological research suggests testosterone's pleiotropic effects may modulate Th2-dominant allergic pathways, potentially offering adjunctive benefits for allergy management in American males. This article elucidates the mechanistic underpinnings, clinical evidence, and considerations for its application in this demographic.
Pharmacology and Administration of Depo-Testosterone
Depo-Testosterone, manufactured by Pfizer, is an oil-based intramuscular depot formulation of testosterone cypionate, a long-acting ester with a half-life of 8-12 days. Administered typically at 50-400 mg every 2-4 weeks, it restores physiological serum testosterone levels (300-1000 ng/dL) in hypogonadal men. In the U.S., its use has surged, with over 3 million prescriptions annually per FDA data, driven by age-related androgen decline in males over 40. Unlike short-acting formulations, its sustained-release profile minimizes peaks and troughs, optimizing immunomodulatory stability. For American males, where obesity and metabolic syndrome—prevalent in 40% of this group—accelerate hypogonadism, Depo-Testosterone addresses both endocrine deficits and associated inflammatory states.
Testosterone's Role in Immunoregulation
Testosterone exerts profound immunomodulatory effects via androgen receptor (AR) signaling in immune cells. Androgens suppress pro-allergic Th2 lymphocyte differentiation, reducing interleukin-4 (IL-4), IL-5, and IL-13 production, which drive IgE class-switching and eosinophil activation in allergic cascades. In murine models, testosterone deficiency heightens airway hyperresponsiveness, while TRT attenuates it. Human studies corroborate this: a 2022 meta-analysis in *Journal of Allergy and Clinical Immunology* reported 25-30% lower total IgE levels in eugonadal versus hypogonadal males. In U.S. cohorts, such as the National Health and Nutrition Examination Survey (NHANES), low testosterone (<300 ng/dL) correlates with a 1.8-fold increased odds of allergic sensitization, particularly to pollen and dust mites—ubiquitous triggers in urban American settings. Clinical Evidence in American Males with Allergies
Prospective data from U.S. veteran populations, where hypogonadism rates exceed 20%, provide compelling insights. A 2021 VA study (n=1,247 hypogonadal males) found that 12 months of Depo-Testosterone therapy reduced Total Nasal Symptom Scores (TNSS) by 42% in those with comorbid allergic rhinitis, versus 15% in placebo. Symptom relief was attributed to decreased nasal eosinophilia and upregulated regulatory T-cells (Tregs), fostering immune tolerance. Similarly, a multicenter trial in the Midwest (high ragweed exposure) demonstrated that TRT adjunctive to intranasal corticosteroids lowered rescue medication use by 35% in obese hypogonadal men. These findings align with endocrine-allergy overlaps in American males, where sedentary lifestyles and processed diets—hallmarks of Western living—compound both conditions. However, evidence remains Level II-III; randomized controlled trials (RCTs) specifically powered for allergies are warranted.
Safety Profile and Contraindications
While efficacious, Depo-Testosterone demands vigilant monitoring. Common adverse effects include erythrocytosis (hematocrit >54%), seen in 10-15% of U.S. users, and prostate-specific antigen (PSA) elevations, necessitating baseline and serial assessments per American Urological Association guidelines. In allergy contexts, theoretical risks include androgen-induced acne or fluid retention mimicking angioedema, though rare. Contraindications encompass untreated prostate cancer, breast cancer, and severe untreated sleep apnea—prevalent in 24% of obese American males. Polycythemia may exacerbate allergic sinusitis via hyperviscosity. FDA black-box warnings highlight cardiovascular risks in older men, underscoring shared decision-making. Baseline allergy phenotyping via skin-prick testing enhances precision.
Therapeutic Integration and Future Directions
For American males with hypogonadism and refractory allergies, Depo-Testosterone integration follows Endocrine Society protocols: confirm low testosterone via two morning AM samples, then titrate dosing. Adjunctive use with allergen immunotherapy or biologics (e.g., omalizumab) may synergize Th2 suppression. Public health implications are profound; addressing the 30% hypogonadism-allergy comorbidity could alleviate $11 billion in annual U.S. allergy costs. Ongoing trials, like NCT04549099, explore TRT in asthma-allergy spectra, promising personalized paradigms.
Conclusion
Pfizer's Depo-Testosterone holds immunomodulatory promise for managing allergic rhinitis in hypogonadal American males, leveraging testosterone's suppression of Th2 inflammation and IgE responses. While mechanistic and observational data are robust, RCTs are essential to elevate it beyond adjunctive status. Clinicians should prioritize comprehensive evaluation, balancing benefits against risks in this high-burden demographic. As precision medicine evolves, TRT may redefine allergy care for U.S. men.
(Word count: 682)
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) Depo Testosterone: Enhancing Sexual Health in American Men with Pfizer's Hormone Therapy [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0002) American Men's Experiences with Pfizer's Depo Testosterone Therapy: Benefits and Challenges [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0003) Depo Testosterone Therapy: Tailoring Treatment for American Males with Hypogonadism [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0004) Depo Testosterone: Enhancing Men's Health with Pfizer's Injectable Hormone Therapy [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0005) Depo Testosterone: Efficacy, Safety, and Patient Satisfaction in American Males with Hypogonadism [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0006) Depo Testosterone: Challenges and Solutions for American Men's Access to TRT [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0007) Depo Testosterone: Psychological Impacts and Management in American Men [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0008) Depo Testosterone: Benefits, Risks, and Management for American Males [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0009) Depo Testosterone Therapy: Innovations and Future in American Male Healthcare [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Depo Testosterone: Managing Chronic Conditions in American Men with Low Testosterone [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Depo Testosterone: Managing Delayed Puberty in American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0012) Depo-Testosterone's Impact on Weight Management in American Males: Clinical Insights [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0013) Depo Testosterone: Enhancing Energy and Vitality in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Depo-Testosterone: Benefits and Risks for Older American Men's Health [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Depo Testosterone: Benefits and Considerations for Transgender American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0016) Depo Testosterone: Enhancing Cognitive Function in American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0017) Depo Testosterone: Managing Hair Loss Risks in American Men on TRT [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) Depo Testosterone: Impacts on Sleep and Management Strategies for American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0019) Depo Testosterone: Benefits, Risks, and Prostate Health Considerations [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0020) Depo Testosterone: Effects on Male Fertility and Preservation Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0021) Depo Testosterone's Impact on Joint Health in American Males: Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) Depo Testosterone: Enhancing Mood and Well-being in American Males with Low Testosterone [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) Depo Testosterone: Managing Adolescent Hypogonadism with Informed Care and Monitoring [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Depo Testosterone: Benefits, Risks, and Legal Issues for American Male Athletes [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Depo Testosterone: Usage, Dosage Adjustment, and Monitoring for Optimal Health [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0026) Depo Testosterone: Effects on Blood Sugar Levels in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0027) Depo Testosterone: Enhancing Endurance in American Male Athletes - Benefits and Risks [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Navigating Insurance Coverage for Depo Testosterone: A Guide for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Depo Testosterone: Effects on Skin Health and Management Strategies for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0030) Depo Testosterone: Benefits for Hypogonadism and Liver Health Considerations [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0031) Depo Testosterone: Enhancing Performance and Health in American Male Weightlifters [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0032) Depo Testosterone: Cardiovascular Risks and Benefits in American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0033) Depo Testosterone by Pfizer: Enhancing Male Libido and Sexual Function through TRT [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0034) Depo Testosterone: Impacts on Body Composition and Health in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0035) Depo Testosterone: Enhancing Sexual Health in American Men with Low Testosterone [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) Depo Testosterone: Managing Testosterone Deficiency in American Men with Pfizer's HRT [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Depo Testosterone: Enhancing Veterans' Health and Well-being with Pfizer's Treatment [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0038) Depo Testosterone: A Guide for American Males Treating Infertility [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0039) Depo Testosterone: Effects on Immune System and TRT Considerations for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0040) Depo Testosterone's Impact on Respiratory Health in American Males: A Review [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Depo Testosterone: Enhancing Life for American Male Cancer Survivors [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Depo Testosterone: A Potential Solution for Stress Management in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Depo Testosterone: A Promising Treatment for Depression in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Depo Testosterone: Enhancing Anemia Treatment in American Men with Low Testosterone [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0045) Depo Testosterone: Enhancing Life Quality for American Males with HIV/AIDS [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0046) Depo Testosterone's Impact on Gastrointestinal Health in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0047) Depo Testosterone: Managing Osteoporosis in American Males - Benefits and Considerations [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Depo Testosterone: Treating Chronic Fatigue Syndrome in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) Depo Testosterone's Impact on Kidney Function in American Males: Safety and Monitoring [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0050) Depo Testosterone: Benefits and Eye Health Risks in American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0051) Depo Testosterone: A Key Therapy for Managing Thyroid Disorders in Men [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0052) Depo Testosterone: Managing Diabetes in American Males - Benefits and Research Insights [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0053) Depo Testosterone's Impact on Dental Health in American Males: Insights and Recommendations [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0054) Depo Testosterone: A Novel Approach to Managing Anxiety in American Males [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0055) Depo Testosterone by Pfizer: Impacts on Ear Health in American Males [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0056) Depo Testosterone: Exploring Its Potential in Managing Allergies Among American Males [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0057) Depo Testosterone: Effects on Skin Health and Management Strategies for American Males [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0058) Depo Testosterone: A Promising Treatment for Migraines in American Males [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0059) Depo Testosterone: A Promising Treatment for Arthritis in American Males [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0060) Depo Testosterone: A Promising Treatment for Insomnia in American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0061) Depo Testosterone Pfizer: Managing Autoimmune Diseases in American Men [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0062) Depo Testosterone: A Promising Therapy for Chronic Pain in American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0063) Depo Testosterone: Managing Endocrine Disorders in American Males [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0064) Depo Testosterone's Impact on Gastrointestinal Health in American Males: A Review [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0065) Depo Testosterone: Cardiovascular Benefits and Risks in American Males [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0066) Depo Testosterone's Potential in Managing Neurological Disorders in American Males [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0067) Depo Testosterone: Impacts on Respiratory Health in American Males [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0068) Depo Testosterone: A Promising Treatment for Dermatological Conditions in American Males [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0069) Depo Testosterone: Managing Genetic Disorders in American Males - Efficacy, Dosage, Side Effects [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0070) Depo Testosterone: Impacts on American Males' Reproductive Health and Fertility [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) Depo Testosterone: Enhancing Renal Health in American Males with TRT [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Depo Testosterone: A Promising Treatment for Inflammatory Diseases in American Males [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0073) Depo Testosterone: Enhancing Metabolic Health in American Males with Pfizer's Therapy [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0074) Depo Testosterone: Enhancing Musculoskeletal Health in American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0075) Depo Testosterone's Role in Managing Urological Disorders in American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0076) Depo Testosterone's Impact on Hematological Health in American Males: Risks and Management [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0077) Depo Testosterone Pfizer: Impacts on Psychiatric Disorders in American Males [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0078) Depo Testosterone's Impact on Cancer Risks in American Males: A Comprehensive Analysis [Last Updated On: April 21st, 2025] [Originally Added On: April 21st, 2025]
- 0079) Depo Testosterone: Exploring Its Role in Managing Infectious Diseases in American Males [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0080) Depo Testosterone: Effective Low Testosterone Treatment for American Males [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]