Is it true that men are more adversely affected by COVID-19?
Yes! And testosterone may be the missing link.
It’s a fact. Men are hit harder than women regarding the devastating effects of the COVID-19 virus. According to the New York City health department, on April 7th, 2020, 2232 men died of the virus in New York City compared to 1,309 women,
More than 40,000 male patients were sick enough from the virus to be hospitalized at that time, compared to around 34,000 women. The city's Coronavirus death rate per 100,000 was 55 men and less than 30 for women.
Fast-forward to August 27th. At that time, the city’s health department concluded that 11,389 men had died of the virus as opposed to 7,646 women.
And it’s not just New York City where this difference occurred
China reported that the COVID-19 mortality rate for men was 2.8% compared to 1.7% for women. Italy declared a similar gap: 72% of deaths from the virus were men, and another study found an even higher number of 80% men dying vs. 20% women...a 4-1 ratio!
 Why is there such a difference in fatalities from the Coronavirus between the genders? Is it that men engage in more reckless behavior, such as not wearing masks, not keeping social distance, smoking and drinking alcohol more than women, and putting off going to the doctor when they are not feeling well?
Why is there such a difference in fatalities from the Coronavirus between the genders? Is it that men engage in more reckless behavior, such as not wearing masks, not keeping social distance, smoking and drinking alcohol more than women, and putting off going to the doctor when they are not feeling well?
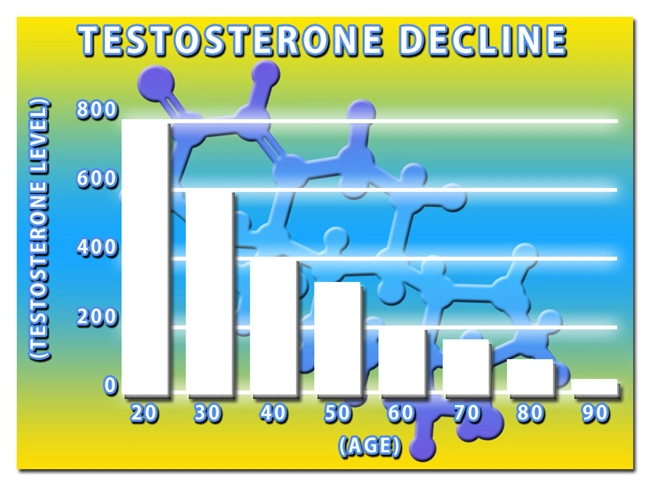
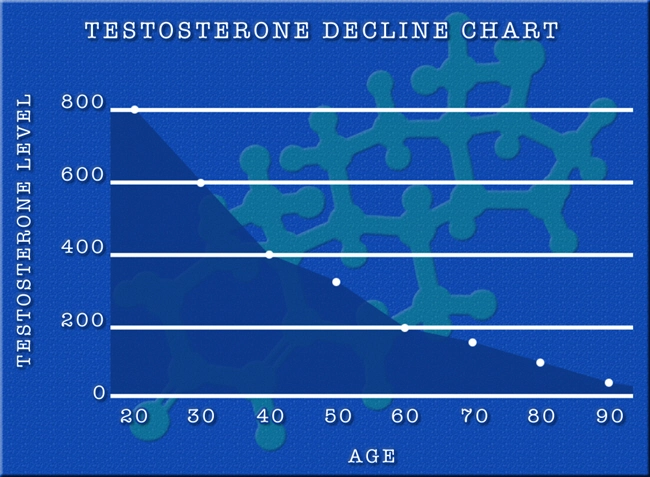
Perhaps. But there may be another answer: the COVID-19 virus may deplete testosterone levels in men, causing a condition called “Low-T.”
To answer that question, let’s take a look at what recent studies have concluded.
In a recent significant study in Turkey on patients hospitalized due to Covid-19, the researchers concluded that the disease might lower men's testosterone levels.
The findings, published in the journal The Aging Male, determined that, as men's testosterone level at baseline plummets, their likelihood of being admitted to the intensive care unit (ICU) significantly increases.
While it has already been reported that low testosterone levels may be linked to a poor prognosis following a positive SARS-CoV-2 test, this is the first study to show that Covid-19 itself lowers testosterone.
Researchers measured levels of 200 men hospitalized after testing positive for Covid-19.
More than half (51 percent) had developed a condition called hypogonadism, in which their bodies did not produce enough testosterone. On average, participants' levels were decimated by 30 percent after the virus hit to marginal unhealthy levels.
Hypogonadism is also called “Low-T.”
"Testosterone is associated with the immune system of respiratory organs, and low levels of testosterone might increase the risk of respiratory infections," said study author Selahittin Cayan from the University of Mersin in Turkey.
"Low testosterone is also associated with infection-related hospitalization and all-cause mortality in the male in ICU patients, so testosterone treatment may also have benefits beyond improving outcomes for Covid-19," she added.
The study consisted of 438 patients. This included 232 males, each with laboratory-confirmed SARS-CoV-2.
All data were prospectively collected. A detailed clinical history, complete physical examination, laboratory, and radiological imaging studies were performed in every patient. All data of the patients were checked and reviewed by the two physicians.
every patient. All data of the patients were checked and reviewed by the two physicians.
Results showed these patients saw their levels drop by a third, on average, from 458 anagrams per deciliter (ng/dl) to 315 ng/dl.
A healthy testosterone level is usually considered to be above 300 ng/dl.
The study was divided into three groups: asymptomatic patients (46), symptomatic patients who were hospitalized in the internal medicine unit (IMU) (29), and patients who were hospitalized in the intensive care unit (ICU) (46). In this study, the mean total testosterone decreased as the severity of Covid-19 increased.
The mean total testosterone level was significantly lower in the ICU than in the asymptomatic group. Also, the mean total testosterone level was significantly lower in the ICU group than in the Intermediate Care Unit group. The mean serum follicle-stimulating hormone level was considerably higher in the ICU group than in the asymptomatic group.
"We found Hypogonadism – a condition in which the body doesn't produce enough testosterone – in 51.1 per cent of the male patients," Cayan said"
“The patients who died had significantly lower mean total testosterone than those who were alive. However, even 65.2 per cent of the 46 asymptomatic male patients had a loss of libido. In our study, the mean total testosterone decreased as the severity of the Covid-19 increased” Cayan added.
Even among men who showed no symptoms of the virus, two-thirds reported having a lowered sex drive, which is a sure sign of low testosterone.
As well as being essential in developing sex organs and muscle growth, testosterone also helps regulate immune responses, including fighting viral infections.
Low levels of the hormone have been linked to an increased risk of dying from the flu, as well as inflammation, heart disease, fatigue, muscle weakness, joint aches and pains, and high blood pressure.
Death was observed in 11 of the male adult patients (4.97%) and 7 of the female patients (3.55%), revealing no significance between the two genders (p?>?0.05).
Commenting on the study results, Professor Çayan added: "It could be recommended that at the time of COVID-19 diagnosis, testosterone levels are also tested. In men with low levels of sex hormones who test positive for COVID-19, testosterone treatment could improve their prognosis. More research is needed on this."
The authors state future studies should look at the concentration levels of ACE2 (Angiotensin-converting enzyme 2) – an enzyme attached to the cell membranes of cells located in the intestines – concerning the total testosterone levels.
In men with low levels of sex hormones who test positive for Covid-19, testosterone treatment could improve their prognosis. More research is needed on this.
The researchers are now calling for all men hospitalized with Covid-19 to have their testosterone levels checked upon admission.
 They say testosterone replacement therapy (TRT) – a relatively safe treatment for men suffering from Low-T – be considered as a treatment option for the virus.
They say testosterone replacement therapy (TRT) – a relatively safe treatment for men suffering from Low-T – be considered as a treatment option for the virus.
Professor Çayan admits the team's study was limited because it did not include a control group of patients with conditions other than Covid-19 to compare with.
She said this was due to the hospital's patient monitoring restrictions. It comes after a study in May found men with low testosterone levels who contract Covid-19 are at far greater risk of dying from the virus.
In another study, medics at the University Medical Center Hamburg-Eppendorf in Germany looked at 45 laboratory-confirmed COVID-19 patients admitted to ICU.
Thirty-five were men, and 10 were women, with seven patients requiring oxygen and 33 needing ventilation. Nine men and three women died.
Each patient's hormone levels were assessed on their first day in ICU before they had received any invasive procedures.
Samples from the COVID-19 patients were tested for 12 hormones, including testosterone and dihydrotestosterone.
Of the male COVID-19 patients sent to ICU at the German hospital, more than two-thirds (68.6 percent) recorded low testosterone levels. In contrast, most female patients (60 percent) had elevated testosterone levels.
In a third study conducted in America, researchers concluded that the Coronavirus might cause men's testicles to swell and lead to infertility. More than a dozen symptoms of COVID-19 have been reported since the pandemic began, including a dry cough, fever, and loss of taste or smell.
Doctors have told men to be extra vigilant of the virus after a 37-year-old patient was taken to A&E with swelling and 'discomfort' in his scrotum.
The patient had already been suffering from the more common signs of COVID, including a cough and fever, for a week before going to the hospital.
Doctors from the San Antonio Uniformed Services Health Education Consortium in Texas said the virus had damaged his spermatocytes, which keep sperm healthy.
 They warned the damage caused by Covid-19 could have a future impact on male fertility.
They warned the damage caused by Covid-19 could have a future impact on male fertility.
Similar reports of testicular pain in Covid-19 patients have been reported previously, but there has been no real research into the link. Doctors who treated him believe the virus entered the body using ACE2 receptors on Leydig cells present in the testes.
Writing in the American Journal of Medicine, they admit that such cases are rare. But they hope raising awareness about them will help other medics 'identify this disease at the earliest junction and trigger appropriate treatment, quarantine, and fertility follow-up.'
The patient spent a night in the hospital before being discharged and prescribed antibiotics and painkillers. His pain is said to have eased slightly, but the case report did not say whether his condition improved in the weeks after.
It is hoped that the development could explain why so many studies have found that male prognosis is worse than those females with COVID-19, and therefore to discover a possible improvement in clinical outcomes using testosterone-based treatments.
The results and conclusions from these studies are a solemn reminder to all men of testosterone's critical role in their overall health. If you are suffering from Low-T, or think you are, contact us for a free, no-obligation discussion.
References
https://www.sciencedaily.com/releases/2020/09/200928125024.htm
https://www.nationalheraldindia.com/health/covid-19-may-deteriorate-mens-testosterone-levels-study
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) Our HGH Clinic And Web Site Privacy Policy [Last Updated On: May 23rd, 2019] [Originally Added On: December 14th, 2017]
- 0002) Idaho HGH Clinics [Last Updated On: August 26th, 2025] [Originally Added On: March 19th, 2018]
- 0003) Injectable HGH Prescriptions In Cheyenne, Wyoming [Last Updated On: April 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0004) Injectable HGH Prescriptions In Milwaukee, Wisconsin [Last Updated On: April 19th, 2025] [Originally Added On: March 3rd, 2019]
- 0005) Injectable HGH Prescriptions In Madison, Wisconsin [Last Updated On: April 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0006) Injectable HGH Prescriptions In Green Bay, Wisconsin [Last Updated On: March 22nd, 2025] [Originally Added On: March 3rd, 2019]
- 0007) Injectable HGH Prescriptions In Charleston, West Virginia [Last Updated On: May 17th, 2025] [Originally Added On: March 3rd, 2019]
- 0008) Injectable HGH Prescriptions In Vancouver, Washington [Last Updated On: February 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0009) Injectable HGH Prescriptions In Tacoma, Washington [Last Updated On: January 16th, 2025] [Originally Added On: March 3rd, 2019]
- 0010) Injectable HGH Prescriptions In Spokane, Washington [Last Updated On: April 16th, 2025] [Originally Added On: March 3rd, 2019]
- 0011) Injectable HGH Prescriptions In Seattle, Washington [Last Updated On: May 30th, 2025] [Originally Added On: March 3rd, 2019]
- 0012) Injectable HGH Prescriptions In Washington D.C [Last Updated On: January 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0013) Injectable HGH Prescriptions In Bellevue, Washington [Last Updated On: June 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0014) Injectable HGH Prescriptions In Virginia Beach, Virginia [Last Updated On: January 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0015) Injectable HGH Prescriptions In Richmond, Virginia [Last Updated On: January 25th, 2025] [Originally Added On: March 3rd, 2019]
- 0016) Injectable HGH Prescriptions In Portsmouth, Virginia [Last Updated On: April 10th, 2025] [Originally Added On: March 3rd, 2019]
- 0017) Injectable HGH Prescriptions In Norfolk, Virginia [Last Updated On: May 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0018) Injectable HGH Prescriptions In Newport News, Virginia [Last Updated On: April 12th, 2025] [Originally Added On: March 3rd, 2019]
- 0019) Injectable HGH Prescriptions In Hampton, Virginia [Last Updated On: January 11th, 2025] [Originally Added On: March 3rd, 2019]
- 0020) Injectable HGH Prescriptions In Chesapeake, Virginia [Last Updated On: January 9th, 2025] [Originally Added On: March 3rd, 2019]
- 0021) Injectable HGH Prescriptions In Arlington, Virginia [Last Updated On: February 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0022) Injectable HGH Prescriptions In Alexandria, Virginia [Last Updated On: May 24th, 2025] [Originally Added On: March 3rd, 2019]
- 0023) Injectable HGH Prescriptions In Montpelier, Vermont [Last Updated On: April 29th, 2025] [Originally Added On: March 3rd, 2019]
- 0024) Injectable HGH Prescriptions In West Valley City, Utah [Last Updated On: April 16th, 2025] [Originally Added On: March 3rd, 2019]
- 0025) Injectable HGH Prescriptions In West Jordan, Utah [Last Updated On: March 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0026) Injectable HGH Prescriptions In Salt Lake City, Utah [Last Updated On: January 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0027) Injectable HGH Prescriptions In Provo, Utah [Last Updated On: May 12th, 2025] [Originally Added On: March 3rd, 2019]
- 0028) Injectable HGH Prescriptions In Wichita Falls, Texas [Last Updated On: April 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0029) Injectable HGH Prescriptions In Waco, Texas [Last Updated On: March 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0030) Injectable HGH Prescriptions In San Antonio, Texas [Last Updated On: February 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0031) Injectable HGH Prescriptions In Round Rock, Texas [Last Updated On: December 29th, 2024] [Originally Added On: March 3rd, 2019]
- 0032) Injectable HGH Prescriptions In Richardson, Texas [Last Updated On: March 10th, 2025] [Originally Added On: March 3rd, 2019]
- 0033) Injectable HGH Prescriptions In Plano, Texas [Last Updated On: February 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0034) Injectable HGH Prescriptions In Pasadena, Texas [Last Updated On: March 31st, 2025] [Originally Added On: March 3rd, 2019]
- 0035) Injectable HGH Prescriptions In Midland, Texas [Last Updated On: April 23rd, 2025] [Originally Added On: March 3rd, 2019]
- 0036) Injectable HGH Prescriptions In Mesquite, Texas [Last Updated On: April 9th, 2025] [Originally Added On: March 3rd, 2019]
- 0037) Injectable HGH Prescriptions In McKinney, Texas [Last Updated On: May 19th, 2025] [Originally Added On: March 3rd, 2019]
- 0038) Injectable HGH Prescriptions In McAllen, Texas [Last Updated On: April 3rd, 2025] [Originally Added On: March 3rd, 2019]
- 0039) Injectable HGH Prescriptions In Lubbock, Texas [Last Updated On: May 10th, 2025] [Originally Added On: March 3rd, 2019]
- 0040) Injectable HGH Prescriptions In Lewisville, Texas [Last Updated On: January 29th, 2025] [Originally Added On: March 3rd, 2019]
- 0041) Injectable HGH Prescriptions In Laredo, Texas [Last Updated On: April 26th, 2025] [Originally Added On: March 3rd, 2019]
- 0042) Injectable HGH Prescriptions In Killeen, Texas [Last Updated On: March 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0043) Injectable HGH Prescriptions In Irving, Texas [Last Updated On: February 9th, 2025] [Originally Added On: March 3rd, 2019]
- 0044) Injectable HGH Prescriptions In Houston, Texas [Last Updated On: April 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0045) Injectable HGH Prescriptions In Grand Prairie, Texas [Last Updated On: January 17th, 2025] [Originally Added On: March 3rd, 2019]
- 0046) Injectable HGH Prescriptions In Garland, Texas [Last Updated On: February 14th, 2025] [Originally Added On: March 3rd, 2019]
- 0047) Injectable HGH Prescriptions In Fort Worth, Texas [Last Updated On: April 21st, 2025] [Originally Added On: March 3rd, 2019]
- 0048) Injectable HGH Prescriptions In El Paso, Texas [Last Updated On: February 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0049) Injectable HGH Prescriptions In Denton, Texas [Last Updated On: May 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0050) Injectable HGH Prescriptions In Dallas, Texas [Last Updated On: December 31st, 2024] [Originally Added On: March 3rd, 2019]
- 0051) Injectable HGH Prescriptions In Corpus Christi, Texas [Last Updated On: June 7th, 2025] [Originally Added On: March 3rd, 2019]
- 0052) Injectable HGH Prescriptions In Carrollton, Texas [Last Updated On: June 3rd, 2025] [Originally Added On: March 3rd, 2019]
- 0053) Injectable HGH Prescriptions In Brownsville, Texas [Last Updated On: February 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0054) Injectable HGH Prescriptions In Beaumont, Texas [Last Updated On: April 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0055) Injectable HGH Prescriptions In Austin, Texas [Last Updated On: June 5th, 2025] [Originally Added On: March 3rd, 2019]
- 0056) Injectable HGH Prescriptions In Arlington, Texas [Last Updated On: January 13th, 2025] [Originally Added On: March 3rd, 2019]
- 0057) Injectable HGH Prescriptions In Amarillo, Texas [Last Updated On: March 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0058) Injectable HGH Prescriptions In Abilene, Texas [Last Updated On: January 5th, 2025] [Originally Added On: March 3rd, 2019]
- 0059) Injectable HGH Prescriptions In Nashville, Tennessee [Last Updated On: March 2nd, 2025] [Originally Added On: March 3rd, 2019]
- 0060) Injectable HGH Prescriptions In Murfreesboro, Tennessee [Last Updated On: March 8th, 2025] [Originally Added On: March 3rd, 2019]
- 0061) Injectable HGH Prescriptions In Memphis, Tennessee [Last Updated On: March 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0062) Injectable HGH Prescriptions In Knoxville, Tennessee [Last Updated On: March 25th, 2025] [Originally Added On: March 3rd, 2019]
- 0063) Injectable HGH Prescriptions In Clarksville, Tennessee [Last Updated On: February 2nd, 2025] [Originally Added On: March 3rd, 2019]
- 0064) Injectable HGH Prescriptions In Chattanooga, Tennessee [Last Updated On: January 29th, 2025] [Originally Added On: March 3rd, 2019]
- 0065) Injectable HGH Prescriptions In Sioux Falls, South Dakota [Last Updated On: December 25th, 2024] [Originally Added On: March 3rd, 2019]
- 0066) Injectable HGH Prescriptions In Columbia, South Carolina [Last Updated On: February 2nd, 2025] [Originally Added On: March 3rd, 2019]
- 0067) Injectable HGH Prescriptions In Charleston, South Carolina [Last Updated On: January 31st, 2025] [Originally Added On: March 3rd, 2019]
- 0068) Injectable HGH Prescriptions In Providence, Rhode Island [Last Updated On: January 30th, 2025] [Originally Added On: March 3rd, 2019]
- 0069) Injectable HGH Prescriptions In Pittsburgh, Pennsylvania [Last Updated On: May 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0070) Injectable HGH Prescriptions In Erie, Pennsylvania [Last Updated On: January 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0071) Injectable HGH Prescriptions In Allentown, Pennsylvania [Last Updated On: May 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0072) Injectable HGH Prescriptions In Salem, Oregon [Last Updated On: January 31st, 2025] [Originally Added On: March 3rd, 2019]
- 0073) Injectable HGH Prescriptions In Portland, Oregon [Last Updated On: February 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0074) Injectable HGH Prescriptions In Gresham, Oregon [Last Updated On: January 30th, 2025] [Originally Added On: March 3rd, 2019]
- 0075) Injectable HGH Prescriptions In Eugene, Oregon [Last Updated On: January 27th, 2025] [Originally Added On: March 3rd, 2019]
- 0076) Injectable HGH Prescriptions In Tulsa, Oklahoma [Last Updated On: May 26th, 2025] [Originally Added On: March 3rd, 2019]
- 0077) Injectable HGH Prescriptions In Oklahoma City, Oklahoma [Last Updated On: February 22nd, 2025] [Originally Added On: March 3rd, 2019]
- 0078) Injectable HGH Prescriptions In Norman, Oklahoma [Last Updated On: April 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0079) Injectable HGH Prescriptions In Toledo, Ohio [Last Updated On: April 14th, 2025] [Originally Added On: March 3rd, 2019]
- 0080) Injectable HGH Prescriptions In Dayton, Ohio [Last Updated On: April 11th, 2025] [Originally Added On: March 3rd, 2019]