The Fascinating link between COVID-19 and Testosterone
COVID-19. The word that most sane people are sick and tired of hearing. COVID-19 Fatigue may be more appropriate.
Few words in recent memory have come with such baggage, and with so many words that we have been bombarded with for so long with seemingly no let-up in sight.
Mask-up...social distancing...lock-downs...variants...new strains...vaccinations...vaccine resistors...Wuhan...censorship...vaccine mandates...political divisions  so entrenched that half of the country does not speak to the other half...the list goes on and on and on.
so entrenched that half of the country does not speak to the other half...the list goes on and on and on.
Regardless of how you feel about the effectiveness and/or safety of the types of COVID vaccines available, virtually everyone agrees that it is better to not have the virus than to have it.
A healthy lifestyle is always our first line of defense from any affliction, including COVID. Nutrition, hydration, fitness, sleep, supplements, and stress control are good ideas under any circumstance, and especially now with COVID hanging around like scenes from a horror movie that just keeps repeating.
But a healthy lifestyle may not stop this monster; more may be needed.
Did you know: Low testosterone levels (“Low-T”) have been found to have a direct connection to COVID-19?
That’s right. A new recent study from Italy concluded that men with low testosterone levels have a significantly greater risk of severe illness and death from COVID-19.
The research included nearly 300 male COVID-19 patients who arrived at the emergency department and were admitted to San Raffaele University Hospital in Milan during the first wave of the pandemic that occurred between February and May of 2020.
The men who were found to have low testosterone following admittance to the hospital were more likely to become severely ill and die from the disease. In fact, they were an incredible six times more likely to die than men with the same disease that were not suffering from Low-T.
they were an incredible six times more likely to die than men with the same disease that were not suffering from Low-T.
Also, the Low-T men had an increased likelihood of needing intensive care, incubation, and longer hospital stays.
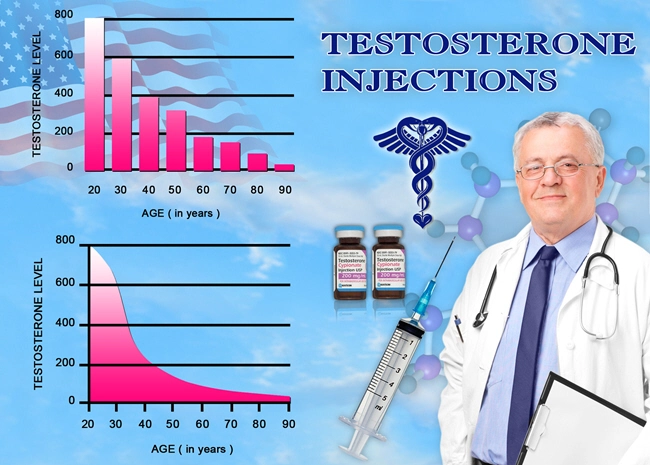
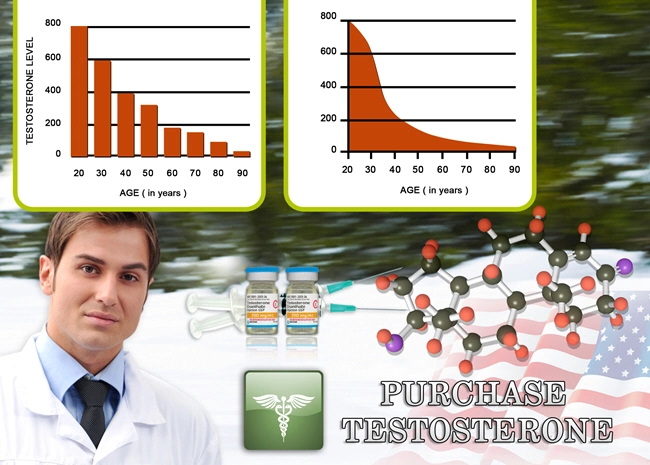
The more severe the illness, the lower the average testosterone level. Here are the numbers:
- Mildly symptomatic and discharged home (3.9 nmol/L)
- Admitted into the internal medicine unit (3.0 nmol/L)
- Admitted to the ICU (1.0 nmol/L)
- Deceased because of COVID-19 (0.7 nmol/L)
"This study outlines that testosterone levels in men with COVID-19 deserve clinical attention, although it remains to be established whether testosterone is simply a marker of health or measuring it may help to target a very high-risk population while establishing counteractive therapeutic measures," reported Paolo  Capogrosso, MD, of Università Vita-Salute San Raffaele in Milan, Italy, during a presentation at the European Association of Urology virtual annual congress.
Capogrosso, MD, of Università Vita-Salute San Raffaele in Milan, Italy, during a presentation at the European Association of Urology virtual annual congress.
"At the start of the COVID pandemic, we were seeing far more men than women coming to the hospital and suffering very severe forms of the disease. We immediately thought this might be related to male hormone levels, particularly testosterone," said the study’s senior author Andrea Salonia, MD, of University Vita-Salute San Raffaele and a urologist at the IRCCS Ospedale San Raffaele.
Salonia then added that "But we never expected to see such a high proportion of COVID patients with these extremely low levels of testosterone, in comparison to a similar group of healthy men. The relationship is very clear: The lower the testosterone, the higher the severity of the condition and likelihood of death. I've never seen anything like it in my 25 years in the field,"
Which came first: COVID-19 or Low-T?
The unexpected results of this study beg the question: are men with low testosterone levels more susceptible to COVID-19 or did the virus lower testosterone in otherwise healthy men? Dr. Salonia stated that the answer to that chicken-or-egg question was uncertain based on the results of the study.
"Testosterone does play a role in protecting men from disease," he said. "However, it's also possible that the virus itself is able to induce an acute reduction in testosterone levels, which then predisposes these men to a worse outcome. We're now following up these patients over a longer time period, to see how their hormone levels change over time, so we can try and answer these questions."
"We simply don't have the data to know which came first in these patients, the low testosterone levels or the COVID," Salonia added.
This was not the only study that established the Low-T/COVID link
Dr. Salonia’s study was one of several studies that discover a connection between low testosterone and COVID-19 severity. In a small study published recently in JAMA Network Open, men with severe COVID-19 had significantly lower levels of testosterone than men with mild cases (53 vs 151 ng/dL).
And a 2020 study in The Aging Male determined that among 221 men hospitalized with COVID-19, low testosterone levels significantly increased the risk of ICU admission and mortality.
The San Raffaele University Hospital study included nearly 300 patients with symptomatic COVID-19 admitted to the emergency department who were compared with 281 healthy men as well as 24 men with asymptomatic COVID-19.
All patients in the study were checked for levels of male hormones, including testosterone, which was considered low if less than 9.2 nmol/L (hypogonadism).
Testosterone is measured in nanomoles per liter (nmol/l) and 9.2 or below is deemed the threshold for low testosterone, termed hypogonadism.
Nearly 90 per cent of the patients had testosterone below this level, compared to just 17 per cent of the healthy volunteers.
Furthermore, testosterone levels in the patients were also significantly below the threshold, averaging around 2.5 nmol/l.
Those patients who had mild symptoms or were admitted to the hospital had slightly higher testosterone levels (between 3-4 nmol/l) than those admitted to ICU or those who died of the disease (just 0.7-1.0 nmol/l).
Even when age, obesity, and pre-existing conditions were factored into the equation, the differences in testosterone levels and COVID recovery were still significant.
The researchers didn't have data on the COVID-19 patients' testosterone levels before they contracted the disease, so they couldn't determine whether low testosterone was a pre-existing condition that made the disease worse or whether the coronavirus infection caused low testosterone.
Data and conclusions presented at meetings should be considered preliminary until published in a peer-reviewed medical journal.
The COVID-19 nightmare is far from over.
Vaccination rates have increased, and the severe, austere lock-downs have been eased, so it is easy to think that the virus is on its last legs, right?
WRONG! The COVID-19 variants and mutations are still surviving in a Rasputin-like manner. The virus seems to keep staggering forward, impervious to our efforts to deliver the final death blow. This is not the time to let our guards down.
Now that you know the proven link between lower testosterone and COVID-19, let’s review the symptoms of Low-T. The American Urology Association (AUA) identifies low testosterone symptoms as the following:
- Low sex drive
- Fatigue
- Reduced lean muscle mass
- Irritability
- Erectile dysfunction
- Depression.
The AUA adds that: "There are many other possible reasons for these symptoms, such as opioid use, some congenital conditions (medical conditions you are born with), loss of or harm to the testicles, diabetes, and obesity (being overweight).
Professor Jens Sonksen, an executive member of the EAU (Europe’s biggest urology conference), said: “The SARS-CoV-2 pandemic has had a tremendous impact on global health since the virus first started spreading in early 2020. We have learned a lot about the virus and possible health consequences from COVID-19 since those early days, but there is much still to learn. "This is highlighted by this new research, which found a surprisingly low level of total testosterone in men with COVID-19 compared to healthy controls.
"Symptomatic COVID-19 patients with low testosterone were also more likely to become critically ill from COVID-19. Additional research on potential impacts from COVID-19 on men’s health is definitely needed.”
And this is where we come in
Our hormone replacement clinics specialize in restoring your testosterone to a more youthful level. Our treatments will have you looking and feeling like you did a few decades ago. The fat will melt, the muscle with firm, and your energy levels will explode and make you feel like living again...not just existing.
 But Testosterone Replacement Therapy (TRT) will do more than give you a more youthful appearance. Read the facts from the studies and let this sink in: low testosterone can make a lifesaving difference in the battle against COVID-19!
But Testosterone Replacement Therapy (TRT) will do more than give you a more youthful appearance. Read the facts from the studies and let this sink in: low testosterone can make a lifesaving difference in the battle against COVID-19!
We have the experience. The know-how. The most modern hormone treatment regimens and technology. You owe it to yourself to add one more barrier to your moat of defenses against this dreaded killer virus.
You don’t need to be a sheep waiting in the slaughter line. Take action as if your life depends on it...because it does!
Contact us for a FREE, no-obligation discussion of the benefits hormone replacement can deliver.
Contact Us Today For A Free Consultation
Dear Patient,
Once you have completing the above contact form, for security purposes and confirmation, please confirm your information by calling us.
Please call now: 1-800-380-5339.
Welcoming You To Our Clinic, Professor Tom Henderson.

- 0001) Our HGH Clinic And Web Site Privacy Policy [Last Updated On: May 23rd, 2019] [Originally Added On: December 14th, 2017]
- 0002) Idaho HGH Clinics [Last Updated On: August 26th, 2025] [Originally Added On: March 19th, 2018]
- 0003) Injectable HGH Prescriptions In Cheyenne, Wyoming [Last Updated On: April 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0004) Injectable HGH Prescriptions In Milwaukee, Wisconsin [Last Updated On: April 19th, 2025] [Originally Added On: March 3rd, 2019]
- 0005) Injectable HGH Prescriptions In Madison, Wisconsin [Last Updated On: April 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0006) Injectable HGH Prescriptions In Green Bay, Wisconsin [Last Updated On: March 22nd, 2025] [Originally Added On: March 3rd, 2019]
- 0007) Injectable HGH Prescriptions In Charleston, West Virginia [Last Updated On: May 17th, 2025] [Originally Added On: March 3rd, 2019]
- 0008) Injectable HGH Prescriptions In Vancouver, Washington [Last Updated On: February 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0009) Injectable HGH Prescriptions In Tacoma, Washington [Last Updated On: January 16th, 2025] [Originally Added On: March 3rd, 2019]
- 0010) Injectable HGH Prescriptions In Spokane, Washington [Last Updated On: April 16th, 2025] [Originally Added On: March 3rd, 2019]
- 0011) Injectable HGH Prescriptions In Seattle, Washington [Last Updated On: May 30th, 2025] [Originally Added On: March 3rd, 2019]
- 0012) Injectable HGH Prescriptions In Washington D.C [Last Updated On: January 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0013) Injectable HGH Prescriptions In Bellevue, Washington [Last Updated On: June 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0014) Injectable HGH Prescriptions In Virginia Beach, Virginia [Last Updated On: January 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0015) Injectable HGH Prescriptions In Richmond, Virginia [Last Updated On: January 25th, 2025] [Originally Added On: March 3rd, 2019]
- 0016) Injectable HGH Prescriptions In Portsmouth, Virginia [Last Updated On: April 10th, 2025] [Originally Added On: March 3rd, 2019]
- 0017) Injectable HGH Prescriptions In Norfolk, Virginia [Last Updated On: May 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0018) Injectable HGH Prescriptions In Newport News, Virginia [Last Updated On: April 12th, 2025] [Originally Added On: March 3rd, 2019]
- 0019) Injectable HGH Prescriptions In Hampton, Virginia [Last Updated On: January 11th, 2025] [Originally Added On: March 3rd, 2019]
- 0020) Injectable HGH Prescriptions In Chesapeake, Virginia [Last Updated On: January 9th, 2025] [Originally Added On: March 3rd, 2019]
- 0021) Injectable HGH Prescriptions In Arlington, Virginia [Last Updated On: February 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0022) Injectable HGH Prescriptions In Alexandria, Virginia [Last Updated On: May 24th, 2025] [Originally Added On: March 3rd, 2019]
- 0023) Injectable HGH Prescriptions In Montpelier, Vermont [Last Updated On: April 29th, 2025] [Originally Added On: March 3rd, 2019]
- 0024) Injectable HGH Prescriptions In West Valley City, Utah [Last Updated On: April 16th, 2025] [Originally Added On: March 3rd, 2019]
- 0025) Injectable HGH Prescriptions In West Jordan, Utah [Last Updated On: March 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0026) Injectable HGH Prescriptions In Salt Lake City, Utah [Last Updated On: January 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0027) Injectable HGH Prescriptions In Provo, Utah [Last Updated On: May 12th, 2025] [Originally Added On: March 3rd, 2019]
- 0028) Injectable HGH Prescriptions In Wichita Falls, Texas [Last Updated On: April 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0029) Injectable HGH Prescriptions In Waco, Texas [Last Updated On: March 15th, 2025] [Originally Added On: March 3rd, 2019]
- 0030) Injectable HGH Prescriptions In San Antonio, Texas [Last Updated On: February 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0031) Injectable HGH Prescriptions In Round Rock, Texas [Last Updated On: December 29th, 2024] [Originally Added On: March 3rd, 2019]
- 0032) Injectable HGH Prescriptions In Richardson, Texas [Last Updated On: March 10th, 2025] [Originally Added On: March 3rd, 2019]
- 0033) Injectable HGH Prescriptions In Plano, Texas [Last Updated On: February 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0034) Injectable HGH Prescriptions In Pasadena, Texas [Last Updated On: March 31st, 2025] [Originally Added On: March 3rd, 2019]
- 0035) Injectable HGH Prescriptions In Midland, Texas [Last Updated On: April 23rd, 2025] [Originally Added On: March 3rd, 2019]
- 0036) Injectable HGH Prescriptions In Mesquite, Texas [Last Updated On: April 9th, 2025] [Originally Added On: March 3rd, 2019]
- 0037) Injectable HGH Prescriptions In McKinney, Texas [Last Updated On: May 19th, 2025] [Originally Added On: March 3rd, 2019]
- 0038) Injectable HGH Prescriptions In McAllen, Texas [Last Updated On: April 3rd, 2025] [Originally Added On: March 3rd, 2019]
- 0039) Injectable HGH Prescriptions In Lubbock, Texas [Last Updated On: May 10th, 2025] [Originally Added On: March 3rd, 2019]
- 0040) Injectable HGH Prescriptions In Lewisville, Texas [Last Updated On: January 29th, 2025] [Originally Added On: March 3rd, 2019]
- 0041) Injectable HGH Prescriptions In Laredo, Texas [Last Updated On: April 26th, 2025] [Originally Added On: March 3rd, 2019]
- 0042) Injectable HGH Prescriptions In Killeen, Texas [Last Updated On: March 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0043) Injectable HGH Prescriptions In Irving, Texas [Last Updated On: February 9th, 2025] [Originally Added On: March 3rd, 2019]
- 0044) Injectable HGH Prescriptions In Houston, Texas [Last Updated On: April 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0045) Injectable HGH Prescriptions In Grand Prairie, Texas [Last Updated On: January 17th, 2025] [Originally Added On: March 3rd, 2019]
- 0046) Injectable HGH Prescriptions In Garland, Texas [Last Updated On: February 14th, 2025] [Originally Added On: March 3rd, 2019]
- 0047) Injectable HGH Prescriptions In Fort Worth, Texas [Last Updated On: April 21st, 2025] [Originally Added On: March 3rd, 2019]
- 0048) Injectable HGH Prescriptions In El Paso, Texas [Last Updated On: February 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0049) Injectable HGH Prescriptions In Denton, Texas [Last Updated On: May 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0050) Injectable HGH Prescriptions In Dallas, Texas [Last Updated On: December 31st, 2024] [Originally Added On: March 3rd, 2019]
- 0051) Injectable HGH Prescriptions In Corpus Christi, Texas [Last Updated On: June 7th, 2025] [Originally Added On: March 3rd, 2019]
- 0052) Injectable HGH Prescriptions In Carrollton, Texas [Last Updated On: June 3rd, 2025] [Originally Added On: March 3rd, 2019]
- 0053) Injectable HGH Prescriptions In Brownsville, Texas [Last Updated On: February 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0054) Injectable HGH Prescriptions In Beaumont, Texas [Last Updated On: April 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0055) Injectable HGH Prescriptions In Austin, Texas [Last Updated On: June 5th, 2025] [Originally Added On: March 3rd, 2019]
- 0056) Injectable HGH Prescriptions In Arlington, Texas [Last Updated On: January 13th, 2025] [Originally Added On: March 3rd, 2019]
- 0057) Injectable HGH Prescriptions In Amarillo, Texas [Last Updated On: March 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0058) Injectable HGH Prescriptions In Abilene, Texas [Last Updated On: January 5th, 2025] [Originally Added On: March 3rd, 2019]
- 0059) Injectable HGH Prescriptions In Nashville, Tennessee [Last Updated On: March 2nd, 2025] [Originally Added On: March 3rd, 2019]
- 0060) Injectable HGH Prescriptions In Murfreesboro, Tennessee [Last Updated On: March 8th, 2025] [Originally Added On: March 3rd, 2019]
- 0061) Injectable HGH Prescriptions In Memphis, Tennessee [Last Updated On: March 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0062) Injectable HGH Prescriptions In Knoxville, Tennessee [Last Updated On: March 25th, 2025] [Originally Added On: March 3rd, 2019]
- 0063) Injectable HGH Prescriptions In Clarksville, Tennessee [Last Updated On: February 2nd, 2025] [Originally Added On: March 3rd, 2019]
- 0064) Injectable HGH Prescriptions In Chattanooga, Tennessee [Last Updated On: January 29th, 2025] [Originally Added On: March 3rd, 2019]
- 0065) Injectable HGH Prescriptions In Sioux Falls, South Dakota [Last Updated On: December 25th, 2024] [Originally Added On: March 3rd, 2019]
- 0066) Injectable HGH Prescriptions In Columbia, South Carolina [Last Updated On: February 2nd, 2025] [Originally Added On: March 3rd, 2019]
- 0067) Injectable HGH Prescriptions In Charleston, South Carolina [Last Updated On: January 31st, 2025] [Originally Added On: March 3rd, 2019]
- 0068) Injectable HGH Prescriptions In Providence, Rhode Island [Last Updated On: January 30th, 2025] [Originally Added On: March 3rd, 2019]
- 0069) Injectable HGH Prescriptions In Pittsburgh, Pennsylvania [Last Updated On: May 18th, 2025] [Originally Added On: March 3rd, 2019]
- 0070) Injectable HGH Prescriptions In Erie, Pennsylvania [Last Updated On: January 4th, 2025] [Originally Added On: March 3rd, 2019]
- 0071) Injectable HGH Prescriptions In Allentown, Pennsylvania [Last Updated On: May 6th, 2025] [Originally Added On: March 3rd, 2019]
- 0072) Injectable HGH Prescriptions In Salem, Oregon [Last Updated On: January 31st, 2025] [Originally Added On: March 3rd, 2019]
- 0073) Injectable HGH Prescriptions In Portland, Oregon [Last Updated On: February 1st, 2025] [Originally Added On: March 3rd, 2019]
- 0074) Injectable HGH Prescriptions In Gresham, Oregon [Last Updated On: January 30th, 2025] [Originally Added On: March 3rd, 2019]
- 0075) Injectable HGH Prescriptions In Eugene, Oregon [Last Updated On: January 27th, 2025] [Originally Added On: March 3rd, 2019]
- 0076) Injectable HGH Prescriptions In Tulsa, Oklahoma [Last Updated On: May 26th, 2025] [Originally Added On: March 3rd, 2019]
- 0077) Injectable HGH Prescriptions In Oklahoma City, Oklahoma [Last Updated On: February 22nd, 2025] [Originally Added On: March 3rd, 2019]
- 0078) Injectable HGH Prescriptions In Norman, Oklahoma [Last Updated On: April 28th, 2025] [Originally Added On: March 3rd, 2019]
- 0079) Injectable HGH Prescriptions In Toledo, Ohio [Last Updated On: April 14th, 2025] [Originally Added On: March 3rd, 2019]
- 0080) Injectable HGH Prescriptions In Dayton, Ohio [Last Updated On: April 11th, 2025] [Originally Added On: March 3rd, 2019]